Edition: Food, Sugar & Industry
28 March, 2026
In The News
Vol 1, Edition 21
Why Is Sugar So Addictive — The Neuroscience Behind the Craving
Sugar addiction is not a character flaw or a lack of willpower. It is a neurochemical process — one the food industry spent decades studying, engineering, and exploiting. Here's what's actually happening in your brain, and why stopping is harder than anyone told you.

Published By: MAP30 Challenge
Authored By: John Shaw
What Happens in Your Brain When You Eat Sugar — A Timeline
What Happens in Your Brain When You Eat Sugar — A Timeline
Sweet receptors activate on the tongue
The brain receives an immediate signal via the vagus nerve. Dopamine begins releasing in the nucleus accumbens before the sugar even reaches the bloodstream.
Blood glucose rises — insulin released
Glucose enters the bloodstream. The pancreas releases insulin. The brain registers a strong dopamine reward signal — the "bliss peak." This is the moment the food industry engineers for.
Dopamine begins to fall
As blood glucose is cleared by insulin, dopamine drops below baseline. The brain registers a motivational deficit — a neurochemical "pull" toward restoring the reward. This is the craving signal forming.
Blood sugar crash — cortisol rises
Insulin overshoots, driving blood glucose below baseline. The brain interprets this as an emergency. Cortisol is released. Cravings for sugar and high-fat foods intensify. Mood drops. Energy drops.
The cycle restarts
The brain generates a strong motivational drive to consume sugar again — to restore dopamine and blood glucose simultaneously. With repeated cycles, dopamine receptors downregulate. More sugar is needed for the same response. Tolerance has developed.
Receptor downregulation — the addiction deepens
Repeated dopamine spikes cause the brain to reduce receptor density as a compensatory response. The same amount of sugar now produces less reward. The cycle repeats at higher and higher consumption levels to achieve the same effect.
In 1966, Frito-Lay launched a campaign that would become one of the most honest accidental admissions in advertising history: 'Bet You Can't Eat Just One.' It was written as a boast. It was, in fact, a precise description of the neurological trap the product had been engineered to create.
The inability to eat just one is not a personal failing. It is the intended outcome of a design process. The food industry has employed teams of food scientists — professionals whose specific job is to engineer products that override the brain's natural satiety signals and compel continued consumption. Understanding that process, and the neuroscience behind it, changes how you think about sugar, processed food, and your own behavior around both.
"You were told you lacked willpower. The truth is you were up against a billion-dollar science operation designed specifically to defeat it."
Why Is Sugar So Addictive — The Dopamine Mechanism
One of the things that shifted my understanding of my own relationship with food was learning that the craving I felt after eating something sweet was not a character flaw — it was a predictable neurochemical response to a stimulus that had been engineered to produce exactly that response. That reframe changed everything about how I approached the problem.
The brain's reward system evolved to reinforce behaviors essential for survival — eating, reproduction, social bonding. When you do something that promotes survival, the brain releases dopamine, a neurotransmitter that creates a sensation of pleasure and signals 'do that again.' This is the mechanism that makes food rewarding.
Sugar triggers a dopamine release in the nucleus accumbens — the brain's primary reward center — that is disproportionate to its nutritional value. Whole foods produce a moderate, brief dopamine response. Refined sugar, particularly in the concentrated forms found in ultra-processed products, produces a sharper, more intense spike. The brain registers this not as 'I ate food' but as 'I did something exceptionally rewarding.'
With repeated exposure, the brain begins to adapt.
Dopamine receptors downregulate — reduce in number and sensitivity — as a compensatory response to overstimulation. This is tolerance. The same amount of sugar now produces a smaller dopamine response than it once did. More is required to achieve the same effect. This is the neurological definition of addiction, and it has been documented in sugar consumption research using the same brain imaging techniques used to study drug addiction.
Researchers offered rats a choice between intravenous cocaine and sweetened water. In 94% of cases, the rats chose sweetened water — even rats that were already addicted to cocaine. The sweet taste reward proved more powerful than the established cocaine reward in the vast majority of subjects. (Lenoir M et al. — PLOS ONE, 2007)
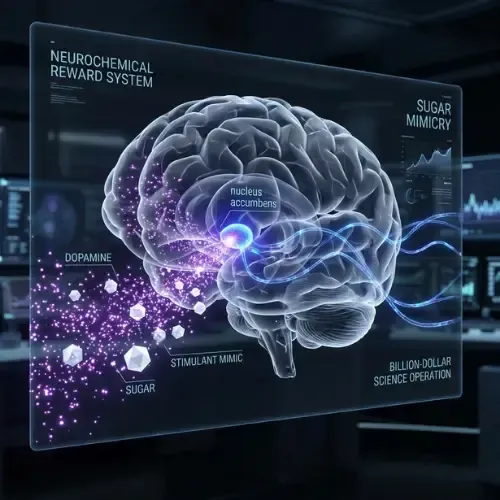
Sugar Addiction Explained: How Food Scientists Engineer the Craving
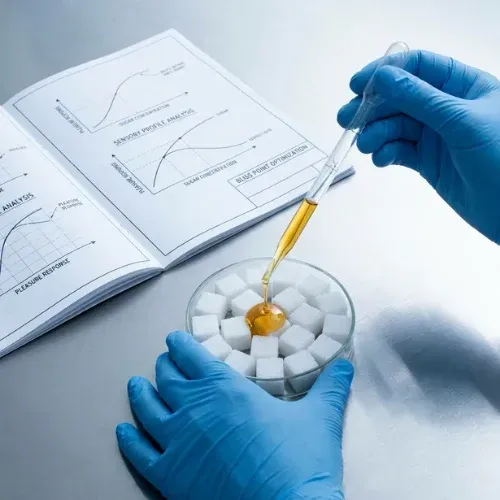
In the 1970s, a food scientist and psychophysicist named Howard Moskowitz developed a concept he called the 'bliss point' — the precise combination of sugar, fat, and salt that maximizes the pleasure response in human subjects. His methodology involved testing hundreds of product formulations on human panels, measuring hedonic response, and identifying the formulation that produced the highest craving without triggering sensory-specific satiety — the brain mechanism that normally signals 'enough.'
Moskowitz's work was initially applied to Pepsi, then spread across the food industry. His insight was not merely that sugar is pleasurable, but that there is a mathematically optimizable level of sweetness that bypasses the brain's off-switch. Too little sugar produces insufficient reward. Too much triggers aversion. The bliss point is the engineered sweet spot that keeps the consumer consuming.
Steven Witherly, a food scientist who spent decades studying hyperpalatable foods — a clinical term for foods engineered to be extraordinarily difficult to stop eating — identified several additional mechanisms beyond sugar. Dynamic contrast (varying textures in the same product), rapid meltdown (foods that dissolve quickly in the mouth, signaling low calorie content to the brain despite high actual caloric density), and sensory-specific satiety suppression through complex flavor layering all contribute to the engineered overconsumption that defines ultra-processed products.
The deliberate engineering of products designed to override satiety signals became the basis of a landmark lawsuit filed on behalf of the People of California against the country's largest food companies.
"The bliss point is not a metaphor. It is a number on a graph — a mathematically calculated formulation designed to make stopping neurologically difficult."
How to Kill Your Sugar Addiction Naturally — Understanding the Craving Cycle
When I started understanding the withdrawal phase of the sugar craving cycle, a lot of my past behavior made sense for the first time. The irritability, the low mood, the urgency I would feel in the afternoon — that was not weakness. That was dopamine falling below baseline and the brain generating a motivational signal to restore it. Understanding it as biology rather than character changed how I navigated it.
The dopamine spike from sugar is followed by a rapid decline — and that decline is the mechanism behind craving. As dopamine falls below baseline after a sugar hit, the brain generates a motivational state oriented toward restoring the reward. This is experienced consciously as craving. The cycle has three phases that repeat in a loop:
1. Binge — consumption of the rewarding substance, dopamine spike, brief satiation
2. Withdrawal — dopamine falls below baseline, anxiety, irritability, low mood
3. Craving — motivational drive to restore dopamine through repeated consumption

This is not metaphorical. This is the same three-phase cycle documented in substance use disorders. Researchers including Bart Hoebel at Princeton and Nicole Avena — whose work on sugar and addiction is among the most cited in the field — demonstrated this cycle in animal models and established that the neurochemical signatures of sugar dependence are functionally identical to those of drug dependence.
A comprehensive review of the neurobiological evidence found that intermittent sugar access produced bingeing behavior, withdrawal symptoms including anxiety and depression when sugar was removed, escalating intake over time, and cross-sensitization with addictive drugs. The authors concluded that sugar meets the behavioral and neurochemical criteria for a substance with addictive potential. (Avena NM, Rada P, Hoebel BG — Neuroscience & Biobehavioral Reviews, 2008)
What 'Bet You Can't Eat Just One' Actually Meant
Frito-Lay's 1966 campaign slogan was, in retrospect, the food industry publicly acknowledging what its internal scientists already knew: that their product had been formulated specifically to defeat the brain's natural stopping mechanism.
The Lay's potato chip formulation at that time had been optimized for several hyperpalatability factors simultaneously: the combination of fat and refined starch produces a calorie-dense substrate that melts quickly in the mouth — a phenomenon food scientists call 'vanishing caloric density' — which delays the brain's fullness signal. Salt amplifies flavor and independently stimulates dopamine release. The crisp texture creates auditory and tactile feedback that heightens the eating experience. The result is a product that delivers intense reward, clears the mouth quickly, and leaves no lasting sense of satiation.
This was not accidental product development. It was the output of a systematic engineering process. The campaign slogan was honest in a way the industry has rarely been since — it named the neurological effect the product had been designed to produce.
"The slogan was the most honest thing the snack food industry ever said. It just took fifty years to understand what it was actually admitting."
Sugar, Insulin, and the Metabolic Consequence
The addiction mechanism operates at the neurological level. The metabolic damage operates at the hormonal level. The two are connected but distinct — and understanding the metabolic consequence of chronic sugar consumption adds a second layer to why the addiction is so difficult to break.
Every time refined sugar is consumed, blood glucose rises sharply and insulin is released to manage it. With frequent sugar consumption, insulin levels remain chronically elevated. Chronically elevated insulin drives fat storage, suppresses fat burning, and over time produces insulin resistance — the condition in which cells stop responding normally to insulin's signal. High-fructose corn syrup — one of the most prevalent forms of added sugar in the processed food supply — routes through the liver rather than the bloodstream, producing liver fat accumulation and insulin resistance through a separate pathway that compounds the damage.
Insulin resistance has a neurological dimension that is rarely discussed. The brain is insulin-sensitive. When insulin signaling in the brain becomes impaired, the normal dopamine regulation that governs reward and satiety is disrupted. Research suggests this impairment both increases the rewarding value of sugar and reduces the brain's ability to generate satisfaction from normal food consumption. The metabolic damage from chronic sugar consumption worsens the neurological trap that drives continued consumption. The two systems reinforce each other.
Research using PET imaging found that obese individuals showed reduced dopamine D2 receptor availability in reward circuits compared to lean controls — the same pattern observed in drug addiction. The reduction correlated with compulsive eating behavior and impaired inhibitory control. Restoring normal glucose metabolism through dietary change partially restored dopamine receptor function. (Volkow ND et al. — Nature Reviews Neuroscience, 2013)
Beating Sugar Addiction — What the Evidence Says Actually Works
Breaking sugar addiction requires understanding that the craving period is neurochemical, not motivational. The discomfort of the first one to two weeks without refined sugar is not a signal that the approach is wrong. It is the brain's dopamine system recalibrating — receptor upregulation, baseline dopamine normalizing, the craving signal losing its urgency as the reward pathway is no longer being overstimulated.
I went through this myself. The first three days were the hardest — the irritability, the low energy, the pull toward something sweet at every dip in the afternoon. By day five it had softened. By week two it had become manageable. What helped me most was understanding that every uncomfortable hour was the brain doing repair work, not evidence that I was failing. Here is what the evidence consistently shows accelerates that recalibration:
1. Protein at every meal — protein blunts the glycemic response, sustains satiety, and reduces the blood sugar volatility that triggers sugar cravings — each meal becomes a stabilization event rather than a spike-and-crash cycle
2. Eliminate liquid sugar first — fruit juice, soda, sweetened coffee drinks, and sports drinks produce the sharpest insulin spikes and fastest dopamine responses. Removing them before addressing solid sugars is the most efficient first step — the change in cravings is often noticeable within days
3. Protect sleep — sleep deprivation increases ghrelin, decreases leptin, and specifically increases cravings for high-sugar, high-fat foods through a cortisol-driven mechanism. Adequate sleep is not optional in sugar addiction recovery — it is a primary lever
4. Use fasting windows — periods of low insulin allow dopamine receptor sensitivity to begin recovering. Even a 12 to 14 hour overnight fast consistently reduces the intensity of sugar cravings within two to three weeks — the fasting window is doing neurological repair work alongside the metabolic reset
The timeline matters. Research on dopamine receptor recovery after cessation of addictive substances consistently shows that the most intense craving period is the first 72 hours. By two weeks, receptor sensitivity has measurably improved. By four weeks, most people report that the craving intensity has substantially decreased. I built the MAP30 framework around exactly this timeline — creating the dietary and fasting conditions that let the biology run its course rather than fighting it with willpower alone. This is not willpower. It is neurobiology running its course.
This article is part of our Food, Sugar & Industry series. Food, Sugar & Industry
Latest Articles

How to Burn Fat
You've been told your body runs on carbohydrates. That's only half the story. Understanding how ketones work in the body — and how to burn fat as fuel...
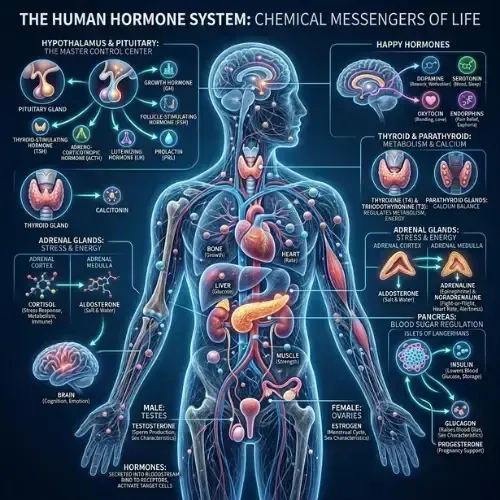
What Are Hormones
Most people think about weight gain as a math problem — calories in versus calories out. The biology is more complex than that.
Fasting and Insulin Resistance
Your A1C came back normal. Your fasting glucose looks fine. Your doctor said everything is okay.

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
FAQ's
1. Is sugar addiction real?
Yes — neurobiologically. Research using brain imaging and animal models has documented that sugar activates the same dopamine reward pathways as addictive drugs, produces tolerance through receptor downregulation, and generates withdrawal symptoms including anxiety and depression when removed. The neurochemical signatures of sugar dependence meet the clinical criteria used to define addiction in substance use disorder research.
2. Why is sugar so addictive?
Sugar triggers a disproportionate dopamine release in the brain's reward center — larger than whole foods produce — and with repeated exposure, dopamine receptors downregulate, creating tolerance. More sugar is required to produce the same reward response. The brain then generates a craving signal when dopamine falls below baseline — the same three-phase binge-withdrawal-craving cycle documented in substance use disorders. The food industry engineered products to exploit this mechanism at its most vulnerable point.
3. What is the bliss point in food science?
The bliss point is the precise combination of sugar, fat, and salt that maximizes the pleasure response without triggering sensory-specific satiety — the brain mechanism that signals fullness. Developed by food scientist Howard Moskowitz in the 1970s and applied systematically across the processed food industry, it is a mathematically calculated formulation designed to keep consumers consuming past the point where whole food would have generated satisfaction.
4. Why can't I stop eating sugar even when I want to?
Because stopping requires overriding a neurochemical craving signal with willpower — a contest that neuroscience consistently shows willpower loses. The craving is generated by dopamine receptor downregulation and blood glucose fluctuations the brain interprets as emergency signals. Until the metabolic environment changes — through reduced sugar intake, stabilized blood glucose, and time for receptor recovery — the craving signal remains physiologically powerful regardless of intention.
5. How long does it take to break a sugar addiction?
The most intense craving period is the first 72 hours after significantly reducing refined sugar. Dopamine receptor sensitivity shows measurable recovery within two weeks. Most people report substantially reduced craving intensity by four weeks of consistent reduced sugar intake. The timeline accelerates with stable blood glucose from adequate protein, adequate sleep, and fasting windows that allow dopamine receptor recovery to proceed without interruption.
6. How addictive is sugar really?
The neurobiological evidence places sugar among the most powerfully rewarding food substances available in the modern diet. In controlled research, sweetness reward has been shown to override established drug addiction in animal models. In human subjects, the dopamine receptor changes associated with chronic high-sugar consumption mirror those documented in substance use disorders. The addictive potential is not colloquial — it is documented through the same research methods used to study drug dependence.
Sources
Lenoir M et al. — 'Intense Sweetness Surpasses Cocaine Reward' (PLOS ONE, 2007) — https://pubmed.ncbi.nlm.nih.gov/17668074/
Avena NM, Rada P, Hoebel BG — 'Evidence for sugar addiction' (Neuroscience & Biobehavioral Reviews, 2008) — https://pubmed.ncbi.nlm.nih.gov/17617461/
Volkow ND et al. — 'Obesity and addiction: neurobiological overlaps' (Nature Reviews Neuroscience, 2013) — https://pubmed.ncbi.nlm.nih.gov/23392215/
Moss M — 'Salt Sugar Fat: How the Food Giants Hooked Us' (Random House, 2013) — https://www.penguinrandomhouse.com/books/209536/salt-sugar-fat-by-michael-moss/
Lustig RH — Journal of the American Dietetic Association, 2010 — https://pubmed.ncbi.nlm.nih.gov/20800122/
Gearhardt AN et al. — Archives of General Psychiatry, 2011 — https://pubmed.ncbi.nlm.nih.gov/21690344/

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
