Edition: Food, Sugar & Industry
24 March, 2026
In The News
Vol 1, Edition 17
Is High Fructose Corn Syrup Bad for You? What Soda Does to Your Liver
The bigger question is not how many calories are in a soda. It is whether high fructose corn syrup is bad for you — and what repeated fructose exposure does inside the liver. Soda delivers a fast, concentrated fructose load that can increase liver fat, raise triglycerides, and worsen insulin resistance over time.

Published By: MAP30 Challenge
Authored By: John Shaw
The Comparison Nobody Makes — But Should
A common claim — repeated by the corn industry and embedded in decades of food labeling — is that high fructose corn syrup is metabolized the same way as regular sugar and poses no unique health risk.
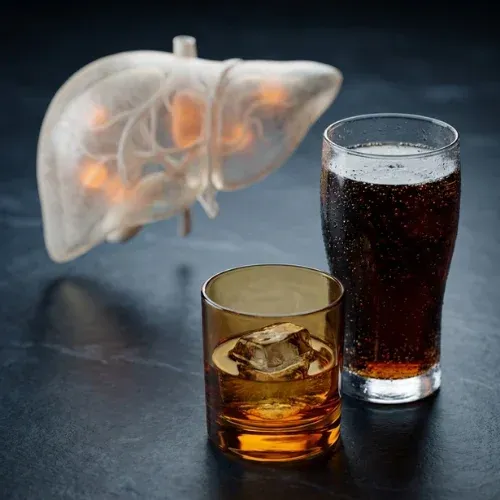
The biochemistry tells a different story. Fructose is processed almost exclusively by the liver, through the same metabolic pathway as alcohol, and in sufficient quantities produces the same downstream consequences: liver fat accumulation, elevated triglycerides, insulin resistance, and inflammation.
Here is a fact that tends to stop people mid-sentence: your liver processes high-fructose corn syrup through nearly the same metabolic pathway it uses to process alcohol. Not a similar pathway. The same one.
The difference between a can of beer and a can of soda, from your liver's perspective, is that one delivers ethanol and one delivers fructose. Both are processed almost exclusively by the liver. Both, in excess, produce the same downstream result: fat accumulation inside liver cells.
Alcohol gets the reputation. Soda gets a pass. That asymmetry is one of the most consequential misunderstandings in modern nutrition — especially for people whose primary goal is losing weight and who are unknowingly working against their own biology every time they reach for a drink they think is harmless.
What "Empty Calories" Actually Means — And Why the Definition Matters

The phrase empty calories has been repeated so often it has lost its meaning. Most people interpret it as "junk food that isn't filling." That interpretation misses the most important half of the definition.
Empty calories means zero nutritional value. No vitamins. No minerals. No fiber. No protein. Just raw energy — and in the case of soda and most sweetened beverages, that energy arrives in the form of high-fructose corn syrup: a highly processed sweetener derived from corn starch that is now one of the most common ingredients in the American food supply.
HFCS is in the obvious places: soda, juice, sweet tea, energy drinks, sports drinks. It is also hiding in places most people would never think to check: ketchup, barbecue sauce, salad dressing, bread, crackers, flavored yogurt, breakfast cereal. Its rise from obscure industrial ingredient to the most common sweetener in the American food supply was enabled by the same era of low-fat dietary guidance that told Americans fat was the enemy and refined carbohydrates were the safe alternative.
this matters because the liver's total daily fructose load is not just what you drink — it is everything that contains HFCS across every meal.
And the total load is what determines the damage.
Why the Liver Is the Problem — The Metabolic Switch
To understand what soda does to your body, you need to understand one fundamental distinction: glucose and fructose are not processed the same way.
Glucose — the most basic form of sugar — is used by virtually every cell in your body. Your muscles burn it for energy. Your brain runs on it. When you consume glucose, it enters the bloodstream, insulin is released, and cells throughout your body absorb and use it. The liver handles some of it, but the workload is distributed.
Fructose is different. It does not trigger the same insulin response. It bypasses the normal satiety signaling that tells your brain you've consumed energy. And critically: it is metabolized almost exclusively by the liver. When fructose arrives, the liver becomes the mandatory processing center for all of it, all at once.
"Think of your liver like a mail sorting facility. Glucose is standard mail — sorted and immediately shipped out to your muscles and organs. Fructose is an unstoppable freight truck that shows up at the loading dock and dumps everything. No distribution. No routing. The liver has to deal with it right there, on the spot. Now imagine that truck showing up three times a day."
This is the metabolic switch that separates soda from almost every other food you might consume. It is not simply "adding calories." It is routing an enormous volume of energy to a single organ that was not designed to handle it in those quantities.
De Novo Lipogenesis: Your Liver's Fat Factory
When the liver receives more fructose than it can immediately use for energy, it does the only thing available to it: it converts the excess into fat. This process has a clinical name - De Novo Lipogenesis- which translates literally from Latin as "making new fat."
This is not a theory or a disputed mechanism. High fructose intake is directly and consistently linked to increased fatty acid synthesis in the liver across a substantial body of peer-reviewed research. The liver's conversion of fructose to fat is well-established metabolic biology.
What happens to that fat matters enormously for your health and your weight:
Some of it is packaged and released into the bloodstream as triglycerides. Elevated triglycerides are an independent risk factor for cardiovascular disease — which is why the research showing a 1.7x cardiovascular disease risk associated with regular HFCS beverage consumption is not surprising to researchers who understand this pathway.
The rest stays in the liver itself, accumulating inside liver cells over time.
The accumulation of fat inside liver cells is the condition known as non-alcoholic fatty liver disease, or NAFLD. A generation ago, this was considered a condition associated with heavy alcohol use, severe obesity, or both. That is no longer accurate. NAFLD is now one of the most common chronic liver diseases in the Western world — affecting an estimated 25 to 30 percent of adults in the United States — and regular consumption of sweetened beverages is consistently identified as one of its primary drivers.
It is showing up in people who do not drink alcohol. In people of normal weight. In people who believe their diet is reasonable. The common variable, again and again, is liquid sugar.
The Domino Effect: Why Liver Fat Is a Fat-Loss Problem, Not Just a Liver Problem
This is where the conversation becomes directly relevant to anyone trying to lose weight — because fat in the liver does not stay contained to the liver.
Fat accumulation in liver cells is not inert. Eliminating ultra-processed food is one of the most direct interventions available — removing the engineered ingredients that drive this cascade simultaneously through multiple pathways. It is metabolically active in ways that disrupt virtually every downstream system involved in weight regulation:
| Intervention | Mechanism and What the Evidence Shows |
|---|---|
| Reduce refined carbohydrates and added sugar | Directly lowers blood glucose variability, reduces ROS production, decreases demand on mitochondrial oxidative phosphorylation, and begins restoring insulin sensitivity. |
| Shift toward fat as a fuel source | When carbohydrate intake decreases and insulin drops, glucagon rises and triggers lipolysis—releasing stored fatty acids that the liver converts to ketones. Ketone metabolism produces fewer ROS and more ATP per unit of substrate. |
| Eliminate ultra-processed foods | Removes the primary dietary source of AGEs, harmful additives, and industrial seed oils associated with mitochondrial damage and systemic inflammation. |
| Time-restricted eating / intermittent fasting | Extending the daily fasting window allows insulin to fall, promotes ketogenesis, triggers cellular autophagy, and supports mitochondrial biogenesis. |
| Exercise — particularly resistance training | Potent stimulus for mitochondrial biogenesis; upregulates PGC-1α. Skeletal muscle is the largest glucose disposal site in the body. |
| Sleep quality | Mitochondrial repair and cellular cleanup occur predominantly during sleep. Chronic sleep deprivation impairs mitochondrial function independently of diet. |
The last two items in that chain are worth dwelling on. Insulin resistance — the direct downstream consequence of sustained liver fat accumulation — is not just a diabetes precursor. It is a fat-loss blocker. When insulin is chronically elevated, the body prioritizes storing energy over burning it. A person with significant insulin resistance can eat at a calorie deficit and still struggle to lose meaningful fat because the hormonal environment is working against the process.
This is the mechanism that explains why many people doing "everything right" — tracking calories, exercising, avoiding obvious junk food — still plateau. The soda, the juice, the daily sweetened coffee drink they did not eliminate is quietly sustaining the liver fat that sustains the insulin resistance that sustains the fat storage.
"A can of soda does not just add empty calories. It is a metabolic event for your liver — one that can trigger a cascade of downstream effects that make fat loss significantly harder, independent of the calories themselves."
The Soda vs. Smoking Comparison — Understanding the Risk
In 2015, a research analysis examining cardiovascular disease risk factors produced a number that researchers in metabolic health found striking: regular consumption of HFCS-sweetened beverages was associated with a cardiovascular disease risk ratio of 1.7. Cigarette smoking, in the same analysis, came in at 1.6.
That comparison is not presented here to suggest soda is more dangerous than smoking in all contexts — the full picture of smoking-related disease is substantially broader. But the cardiovascular number illustrates something important: the metabolic consequences of regular sweetened beverage consumption are not in a minor-indulgence category. They are in a significant-chronic-risk category.
The mechanism is the one described above: fructose overload in the liver, conversion to triglycerides, release into the bloodstream, and sustained elevation of cardiovascular risk markers. The damage is real, it is measurable, and it accumulates over time in the same way any chronic health risk does.
The "But It's Just a Little Sugar" Problem
The most persistent obstacle to changing behavior around sweetened drinks is the perception that the amount involved is trivial. "It's just one soda." "At least I'm not eating fast food." "It's diet anyway."
The fructose metabolism pathway does not scale the way those rationalizations do. Even moderate daily fructose intake, sustained consistently over months and years, produces the liver fat accumulation described above. The research on NAFLD does not show a threshold below which daily HFCS consumption is without consequence. It shows a dose-dependent relationship: more fructose, more liver fat, more downstream disruption.
The other aspect of this that gets overlooked: liquid sugar is categorically different from solid food containing the same amount of sugar. When fructose is consumed in liquid form, it hits the liver faster, in higher concentration, and with none of the buffering effects that fiber and chewing provide with solid food. There is no satiety signal. There is no slowdown in absorption. The truck hits the loading dock at full speed.
This is why eliminating sweetened drinks — not just reducing them, but eliminating them as a daily habit — consistently produces metabolic improvements that calorie math alone would not predict.

The companies that built their product lines around HFCS while downplaying its metabolic consequences are now facing a landmark lawsuit filed on behalf of the People of California, alleging they knowingly engineered addiction and hid the science.
The Label Reading Problem: Where HFCS Hides
One of the reasons daily fructose load is higher than most people realize is that HFCS appears in products that do not read as "sweet" in any meaningful way. Awareness of where it hides is a practical prerequisite to actually reducing it.
Condiments: ketchup, barbecue sauce, relish, sweet chili sauce
Dressings: most commercial salad dressings, especially low-fat varieties
Bread: many commercial sandwich breads and burger buns
Crackers and snack foods: even savory varieties often contain HFCS
Flavored dairy: yogurt, flavored milk, coffee creamers
Breakfast foods: cereals, granola bars, flavored oatmeal packets
Canned goods: baked beans, canned fruit in syrup, some soups
The practical implication: even someone who has stopped drinking soda may still be consuming significant daily HFCS if they are not reading labels across the full range of packaged foods they consume. The liver's total daily fructose load matters — not just what comes in a can.
A Note on "Natural" Sugar — The Table Sugar Comparison
A common response to the concern about HFCS is to reach for cane sugar, honey, or fruit juice instead, under the assumption that "natural" sugar is meaningfully different.
The metabolic reality is more nuanced than that framing suggests. Table sugar — sucrose — is a molecule composed of 50% glucose and 50% fructose. HFCS is 55% fructose and 45% glucose. The difference is five percentage points. The body breaks down both through the same pathways, and the liver's fructose processing is identical regardless of whether the fructose arrives via sucrose or HFCS.
The distinction that matters is not the source. It is the quantity and frequency. A small amount of fructose from whole fruit, which comes packaged with fiber, water, and micronutrients that slow its absorption, is metabolically very different from a large quantity of fructose in liquid form. The fruit does not produce the same loading dock problem. The juice — which removes the fiber and concentrates the fructose — does.
"The question is not whether HFCS or cane sugar is worse. The question is: how much fructose is your liver processing every single day, and in what form? That is the number that matters."
What to Actually Do With This Information
Understanding the mechanism is not the same as having a plan. Here is what the research on liver fat, insulin resistance, and HFCS-driven metabolic dysfunction consistently points toward:
| Dietary Factor | Effect on Insulin and Metabolic Health |
|---|---|
| Refined carbohydrates | Rapid glucose absorption → large insulin spike; chronically elevated insulin demand over time. |
| Added sugar and HFCS | Fructose processed by the liver via de novo lipogenesis → increased liver fat → worsens hepatic insulin resistance. |
| Ultra-processed foods | Engineered for rapid absorption; often combine refined carbs and fats in ratios that maximize insulin response and override satiety signaling. |
| Dietary fiber | Slows glucose absorption → blunts insulin response → supports insulin sensitivity over time. |
| Protein | Minimal direct insulin impact; supports muscle mass, the primary site of glucose disposal. |
| Healthy fats | Lowest glycemic impact of any macronutrient; associated with improved insulin sensitivity in clinical research. |
These are not quick fixes. The liver fat that accumulates over years of regular HFCS consumption does not reverse in a week. But the research on NAFLD is consistent: meaningful dietary changes — particularly the reduction of liquid fructose — produce measurable improvements in liver health, insulin sensitivity, and fat loss over time.
The Bottom Line
Your liver performs over 500 functions to keep you alive every day. It filters your blood, regulates your hormones, manages your energy storage, produces bile for digestion, and processes nearly everything you consume. When it is compromised — when its cells are packed with fat and inflamed and insulin-resistant — all of those functions degrade together.
Soda, juice, and sweetened drinks are not just empty calories. They are the primary delivery mechanism for the fructose that drives liver fat accumulation, insulin resistance, and the downstream metabolic environment that makes fat loss harder regardless of what else you do right.
You cannot out-exercise a daily fructose load that is overwhelming your liver. You cannot out-calorie-count an insulin environment that keeps your body locked in fat storage mode. The drinks have to go first.
"Stop treating soda like a harmless habit and start treating it like what the research shows it to be: a daily metabolic stressor with documented consequences for liver health, cardiovascular risk, and your body's ability to lose fat. The label on the can is not the whole story. The story is what happens inside."
⚠ Disclaimer
The information in this article is for educational purposes only and does not constitute medical advice. If you have concerns about liver health, insulin resistance, or any metabolic condition, consult a qualified healthcare provider before making changes to your diet or health management plan. Individual results vary.
Key references: Stanhope KL, "Sugar consumption, metabolic disease and obesity: The state of the controversy" (Critical Reviews in Clinical Laboratory Sciences, 2016); Lustig RH et al., "Isocaloric fructose restriction and metabolic improvement in children with obesity and metabolic syndrome" (Obesity, 2016); Younossi ZM et al., "Global epidemiology of nonalcoholic fatty liver disease" (Hepatology, 2016); American Heart Association, "Added Sugars and Cardiovascular Disease Risk in Children" (Circulation, 2016); Tappy L & Le KA, "Metabolic Effects of Fructose and the Worldwide Increase in Obesity" (Physiological Reviews, 2010).
This article is part of our Food, Sugar & Industry series. Food, Sugar & Industry
Latest Articles
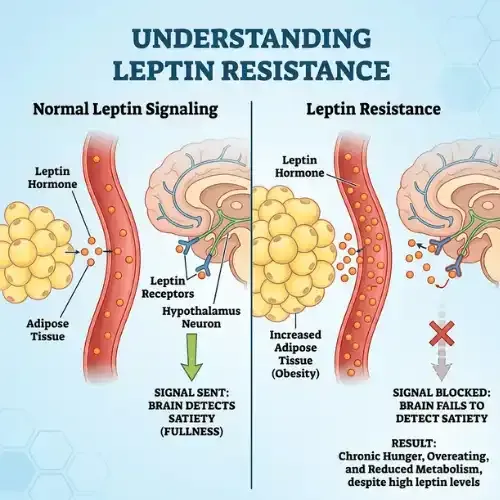
How Leptin Works
Leptin is the hormone your fat cells use to tell your brain you have enough stored energy. When it works, hunger is manageable and weight regulates itself...

Ghrelin - The Hunger Hormone
Ghrelin is the hormone your stomach sends to your brain when it wants you to eat. Understanding how ghrelin works, why it spikes after dieting, and how to reduce ghrelin...

Insulin Blocks Fat Burning
Your body is not broken. It is doing exactly what elevated insulin tells it to do — storing fat and refusing to release it. Understanding the insulin switch is the difference between...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
Disclaimer: The information in this article is for educational purposes only and does not constitute medical advice. Fatigue and related symptoms can have many causes, some of which require medical evaluation and treatment. Nothing in this article should be interpreted as a recommendation to change, stop, or start any medication or treatment plan. Always consult a qualified healthcare provider before making significant changes to your diet or lifestyle..
FAQ's
1. What is high fructose corn syrup?
HFCS is a corn-derived sweetener that typically contains about 42% to 55% fructose, with the rest mostly glucose. It is chemically similar to table sugar, but it is widely used in sweetened beverages and processed foods that make high intake easy.
2. Is high fructose corn syrup bad for you?
High fructose corn syrup can contribute to health problems when consumed regularly in large amounts. The main concern is the fructose content — your liver processes fructose differently from glucose, and high fructose intake from sweetened beverages is linked to liver fat accumulation, elevated triglycerides, and insulin resistance over time. The evidence suggests that the bigger issue is not HFCS specifically, but the total amount of fructose you consume — and sweetened beverages make that amount easy to exceed. Moderate, occasional consumption is unlikely to cause harm, but regular high intake, particularly from drinks, is associated with metabolic consequences.
3. Is high fructose corn syrup worse than regular sugar?
HFCS and table sugar are chemically similar — both contain roughly equal amounts of fructose and glucose. The practical difference at the molecular level is not significant enough to meaningfully distinguish one from the other metabolically. What matters is the total amount of fructose your liver has to process, and how quickly it arrives. Sweetened beverages and processed foods make it easy to consume large amounts of fructose rapidly, and the liver bears most of that load regardless of whether the source is HFCS or cane sugar. Excess fructose intake — not the specific sweetener — is the central issue.
4. What does fructose do to the liver?
Fructose is metabolized primarily in the liver, unlike glucose which is distributed throughout the body. When the liver receives more fructose than it can use for energy, it converts the excess to fat through de novo lipogenesis. This fat can accumulate as non-alcoholic fatty liver disease (NAFLD). Fatty liver is associated with hepatic insulin resistance — the liver stops responding to insulin's signal to suppress glucose production, which can elevate fasting blood glucose and contribute to systemic insulin resistance over time.
5. Does high fructose corn syrup cause insulin resistance?
Excess intake of HFCS-rich beverages can contribute to insulin resistance, in part through liver fat accumulation and higher triglycerides. When the liver accumulates fat from high fructose intake, it may stop responding to insulin normally. The pancreas compensates by producing more insulin, and chronically elevated insulin levels can create an environment where the body has a harder time accessing stored fat for energy. Research supports a dose-dependent relationship between high fructose beverage consumption and metabolic dysfunction, including insulin resistance.
6. What foods contain high fructose corn syrup?
HFCS is found in soft drinks, fruit juices, sweetened teas, energy drinks, bread, breakfast cereals, yogurt, ketchup, salad dressings, candy, cookies, crackers, and most processed snack foods. It is one of the most widely used sweeteners in the US food supply because it is less expensive than sucrose and blends easily into liquid and semi-liquid products. Reading ingredient labels and avoiding products that list HFCS, corn syrup, or corn sweetener in the first five ingredients is the most direct way to reduce intake.
Sources
1. Stanhope KL et al. — "Consuming fructose-sweetened, not glucose-sweetened, beverages increases visceral adiposity"
(Journal of Clinical Investigation, 2009) — https://pubmed.ncbi.nlm.nih.gov/19381015/
2. Lustig RH et al. — "Fructose: metabolic, hedonic, and societal parallels with ethanol" (JAGS, 2010) —
https://pubmed.ncbi.nlm.nih.gov/20414826/
3. Tappy L & Lê KA — "Metabolic effects of fructose and the worldwide increase in obesity" (Physiological Reviews, 2010) —
https://pubmed.ncbi.nlm.nih.gov/20219980/
4. Bray GA et al. — "Consumption of high-fructose corn syrup in beverages may play a role in the epidemic of obesity"
(AJCN, 2004) — https://pubmed.ncbi.nlm.nih.gov/15051594/
5. Malik VS et al. — "Sugar-sweetened beverages and risk of metabolic syndrome and type 2 diabetes" (Diabetes Care,
2010) — https://pubmed.ncbi.nlm.nih.gov/20693348/
6. [ADDED per audit] Harvard T.H. Chan School of Public Health — "High-Fructose Corn Syrup or Table Sugar: For Better
Health, Avoid Too Much of Either" — https://hsph.harvard.edu/news/high-fructose-corn-syrup-or-table-sugar-for-better-
health-avoid-too-much-of-either/
7. [ADDED per audit] PMC Review — "Fructose and Metabolic Health" —

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
