Edition: Weight Loss & Fat Burtning
25 March, 2026
In The News
Vol 1, Edition 18
How to Burn Fat — Why Fat Is Your Body’s Preferred Fuel and How to Access It
You've been told your body runs on carbohydrates. That's only half the story. Understanding how ketones work in the body — and how to burn fat as fuel — changes everything about how you think about energy, hunger, and weight loss.

Published By: MAP30 Challenge
Authored By: John Shaw
Picture this. You eat a full meal. An hour and a half later, you're hungry again. Not peckish — actually hungry. You just ate. There is food in your body. And yet the signal your brain is sending is unmistakable: feed me.
If that sounds familiar, it isn't a willpower problem. It isn't a discipline problem. It is a fuel problem. To understand how to burn fat effectively — and why most people never do — you first need to understand how ketones work in the body, and why the fuel your body was designed to run on is probably not the one it's currently using.
Your body can run on two fuels. Most people only ever use one.
The Two Fuels Your Body Can Burn
The first fuel is glucose — derived from carbohydrates. The second is fat — your body's own stored fat, converted into ketones and burned by your mitochondria. Both are real, both are functional, but they behave very differently inside your body.
The reason most people never tap into fat as a primary fuel is not biological. It's dietary. A diet high in refined carbohydrates and processed foods keeps insulin chronically elevated — and elevated insulin locks the door to your fat stores. The glucose system stays dominant by default, not by design.
“Your body can run on two fuels. Most people only ever use one — not because the other doesn't work, but because the foods they're eating never give it a chance.”
Fuel One: Glucose
Glucose is short-term, fast-burning fuel. When you eat carbohydrates, they break down into glucose, enter your bloodstream, and your cells either use it immediately for energy or store it as glycogen in your liver and muscles.
The problem is the storage capacity. Your liver holds roughly 100 grams of glycogen. Your muscles hold about 400 grams. Total glycogen capacity: approximately 2,000 calories. That's your entire glucose reserve — a few hours of energy at most, depending on activity level.

The other problem is what happens when that glucose hits your bloodstream. Blood sugar rises. Insulin is released in response. And during that spike, insulin's primary job is to move glucose into cells and stop fat burning entirely. You cannot burn stored fat and have elevated insulin at the same time. The two states are mutually exclusive.
Think of glucose as kindling. It burns hot and fast, generates quick energy, but it burns out quickly and needs to be constantly replenished. Every few hours, the fire dies down and hunger pulls you back to the grocery store — even if your fat cells are full.
THE GLUCOSE PROBLEM AT A GLANCE
Spikes blood sugar → triggers insulin → shuts off fat burning
Storage limited to ~2,000 calories (liver + muscles)
Produces only 32 ATP molecules per glucose molecule
Leads to energy crashes and hunger cycles every 2–3 hours
Cannot be burned alongside stored fat while insulin is elevated
Fuel Two: Fat and Ketones
Fat is long-term, stable, clean-burning fuel. Here is how the pathway works: dietary fat and stored body fat break down into fatty acids. Those fatty acids travel to the liver, where they are converted into ketones. The ketones are then delivered to the mitochondria in your cells — your cellular power plants — and burned for energy.
The storage capacity comparison is not even close. Even a lean adult carries 40,000 or more calories of stored fat. That is not a rounding error — it is a reserve twenty times larger than your entire glycogen system. And unlike glycogen, fat storage capacity is virtually unlimited.
The energy yield is also significantly higher. One gram of fat contains 9 calories versus 4 for carbohydrates. More importantly, fat produces 129 ATP molecules per palmitate molecule. Glucose produces 32 ATP per molecule. Fat-burning mitochondria are more efficient cellular engines.

“Even a lean adult carries 40,000+ calories of stored fat. That's not a reserve — that's a fuel tank. The only question is whether insulin is high enough to keep the door locked.”
And critically: fat metabolism does not produce the insulin spikes that glucose does. When insulin is low, your body is free to access its stored fat. The hunger signal that drives you back to eating every few hours quiets down. Energy stabilizes. The relentless cycle of spike, crash, and crave begins to break.
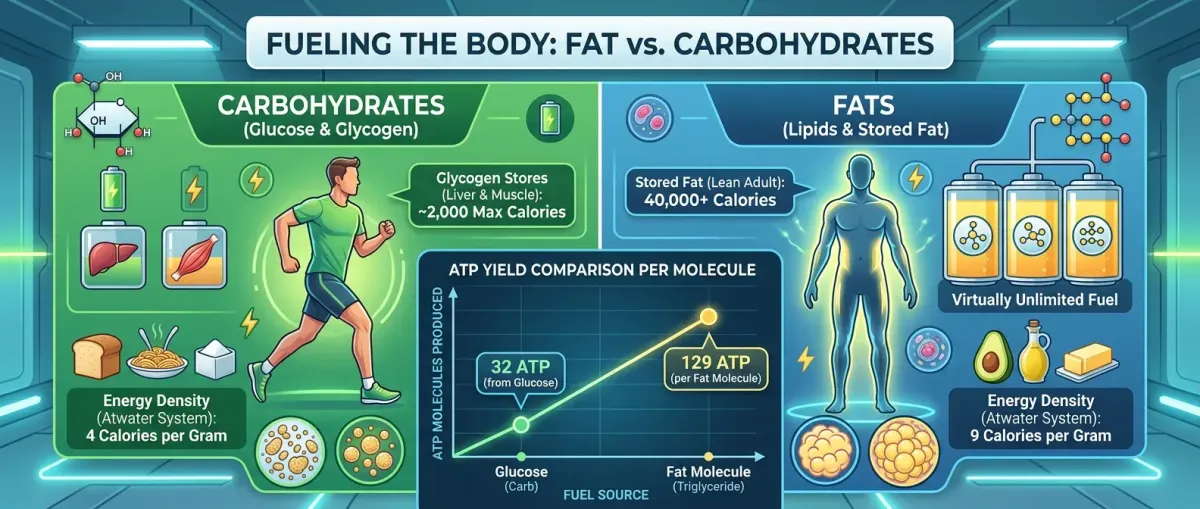
| Glucose (Carbohydrates) | Fat / Ketones |
|---|---|
| Burns fast — depleted in hours | Burns slowly — virtually unlimited supply |
| ~2,000 calories max in storage | 40,000+ calories in a lean adult |
| 32 ATP per glucose molecule | 129 ATP per palmitate molecule |
| Spikes insulin → blocks fat burning | Low insulin response → fat burning enabled |
| Hunger returns every 2–3 hours | Stable energy for 4–6+ hours between meals |
| Energy crashes and cravings | Steady energy, reduced hunger |
| 4 calories per gram | 9 calories per gram |
Why Your Fat Stores Stay Locked

Here is a way to think about what elevated insulin is actually doing to your body.
Imagine you go to the grocery store, buy food, cook dinner, and put the leftovers in the refrigerator. But then you put a lock on the fridge — a lock you can only open to put food in, never to take food out. When you get hungry an hour later, you can't access the food that is right there. You have to go back to the store.
That is insulin. When insulin is chronically elevated, your fat cells are open for deposits but closed for withdrawals. Calories go in; they don't come out. Your stored fat — tens of thousands of calories of available energy — is sitting right there, locked behind a hormonal door you've inadvertently bolted shut.
When insulin stays low — because you've stopped spiking it with refined carbohydrates and processed food — the lock opens. Your body accesses its own stored fat. You burn it for fuel. You lose weight not because you're eating less and suffering for it, but because your body has finally been given permission to use the energy it's been hoarding.
The Broken Signal Between Your Fat Cells and Your Brain
Your body has an elegant communication system built in. Fat cells produce a hormone called leptin, which travels to the brain to signal: we have plenty of stored energy, reduce hunger. When this system is working properly, as fat stores fill up, appetite naturally decreases.
When insulin is chronically elevated, this signaling breaks down. The brain stops receiving the leptin signal accurately — a state called leptin resistance. Your brain thinks you're starving, even when your fat cells are full. So it does what it's designed to do when it thinks starvation is happening: it cranks up ghrelin, the hunger hormone, and drives you toward food.
This is why hunger on a high-carbohydrate diet is not a discipline problem. You are fighting your own biology — a biology that has been disrupted by the foods you're eating. When you stop spiking insulin and restore the leptin signal, hunger decreases naturally. Not because you're exercising more willpower. Because your brain is finally getting accurate information.
THE HORMONAL CHAIN REACTION
High-carb meal → blood sugar spikes
Pancreas releases insulin → fat burning shuts off
Fat cells locked → stored energy inaccessible
Leptin signal disrupted → brain thinks you're starving
Ghrelin rises → hunger intensifies
Blood sugar crashes → cravings for fast carbs return
Cycle repeats
How to Transition to Fat Burning
Becoming a fat burner is not a dramatic intervention. It is a process of removing the foods that keep insulin elevated and giving your body's existing machinery the conditions it needs to shift fuels. Here is how that transition works.
1
Reduce Refined Carbohydrates
Processed foods, sugars, grains, cereals, and anything with a long ingredient list are the primary drivers of chronic insulin elevation. Cutting these — and replacing them with whole foods: meat, eggs, dairy, healthy fats, low-carb vegetables — is step one. When you stop spiking insulin, you start getting gradual rises and falls rather than sharp spikes and crashes. Hunger begins to shift.
2
Increase Healthy Fats
Eating fat does not make you fat — dietary fat has a low glycemic response and does not spike insulin. Fatty cuts of meat, butter, eggs with the yolk, olive oil, and avocado signal to your body that fat is available as fuel. Satiety increases. The time between meals when you genuinely feel satisfied begins to extend.
3
Give Your Mitochondria Time
Your mitochondria need weeks — sometimes months — to upregulate the fat-burning enzymes required to efficiently run on ketones. The transition period can feel uncomfortable: low energy, brain fog, irritability. This is sometimes called the "keto flu" and it is temporary. Metabolic dysfunction built over years takes weeks to begin reversing, but it reverses faster than most people expect.
4
Let Intermittent Fasting Happen Naturally
Intermittent fasting is not starvation. It is simply extending the time between meals — which happens naturally when hunger decreases as fat burning improves. When your body is efficiently accessing stored fat for fuel, going five or six hours between meals without hunger is not an act of willpower. It is what metabolic health feels like.
What Fat Burning Actually Feels Like
The shift from glucose dependence to metabolic flexibility — the ability to comfortably burn fat as a primary fuel — produces changes that are difficult to describe until you experience them.
Energy stabilizes. The mid-afternoon crash, the need for caffeine to close the gap between lunch and dinner, the brain fog that sets in a few hours after eating — these are symptoms of glucose dependence and the insulin roller coaster. They tend to disappear as fat burning improves.
Hunger changes character. Instead of the urgent, sharp hunger that follows a blood sugar crash, appetite on a fat-burning metabolism feels different — slower to arrive, easier to tolerate, more easily managed. Eating becomes a choice rather than an emergency.
Cravings for refined carbohydrates decrease. This is not willpower. When insulin stays low and the leptin-ghrelin signaling system is functioning properly, the biological pull toward sugar and processed carbohydrates diminishes because the hormonal demand that created it has been reduced.
“The goal is not to be thin. The goal is to be metabolically functional — a body that can access its own stored energy, regulate its own hunger, and generate steady fuel without constant feeding.”
The Bigger Picture: What Your Body Was Designed to Do
Human metabolism evolved over hundreds of thousands of years in an environment without refined carbohydrates, without processed food, and without continuous access to food. The ability to store fat efficiently and burn it when food was scarce was not a metabolic flaw — it was the primary survival mechanism.
The past fifty years of carbohydrate-dominant nutrition advice represents a historical anomaly, not a metabolic truth. The obesity epidemic, the insulin resistance epidemic, the metabolic syndrome epidemic — these are the downstream consequences of a food environment that has systematically locked the door to fat burning while continuously refilling the glucose tank.
Restoring metabolic health does not require anything exotic. It requires removing the foods that keep insulin chronically elevated and giving the body's existing fat-burning machinery the conditions it needs to function as it was designed to.
Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Individual metabolic responses vary. Consult a qualified healthcare provider before making significant changes to your diet, especially if you have diabetes, cardiovascular disease, or any other metabolic condition.
References
Cahill GF — "Fuel Metabolism in Starvation" (Annual Review of Nutrition, 2006) — https://pubmed.ncbi.nlm.nih.gov/16848698/
Paoli A et al. — "Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets" (European J Clinical Nutrition, 2013) — https://pubmed.ncbi.nlm.nih.gov/23801097/
Westman EC et al. — "Low-carbohydrate nutrition and metabolism" (Am J Clin Nutr, 2007) — https://pubmed.ncbi.nlm.nih.gov/17684196/
Hall KD et al. — "Energy expenditure and body composition changes after an isocaloric ketogenic diet" (Am J Clin Nutr, 2016) — https://pubmed.ncbi.nlm.nih.gov/27385608/
Lustig RH — "Fructose: It's Alcohol Without the Buzz" (Advances in Nutrition, 2013) — https://pubmed.ncbi.nlm.nih.gov/23408191/
This article is part of our Weight Loss & Fat Burning series. Weight Loss & Fat Burning
Latest Articles

Insulin Blocks Fat Burning
Your body is not broken. It is doing exactly what elevated insulin tells it to do — storing fat and refusing to release it. Understanding the insulin switch is the difference between...

High Fructose Corn Syrup
The bigger question is not how many calories are in a soda. It is whether high fructose corn syrup is bad for you — and what repeated fructose exposure does inside the liver...

What Is Ghrelin
Ghrelin is the hormone your stomach sends to your brain when it wants you to eat. Understanding how ghrelin works, why it spikes after dieting, and how to reduce ghrelin...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
FAQ's
1. How does fat burning work?
Fat burning — technically called lipolysis and beta-oxidation — is the process by which the body breaks down stored triglycerides into free fatty acids and glycerol, then transports those fatty acids to the mitochondria where they are oxidized for energy. This process is directly regulated by insulin: when insulin is low, fat burning proceeds. When insulin is elevated, the enzyme that initiates lipolysis (hormone-sensitive lipase) is suppressed and fat burning stops.
2. Why is fat the body’s preferred fuel?
Fat is the most energy-dense macronutrient, providing nine calories per gram versus four for carbohydrates. More importantly, the body stores virtually unlimited fat but only a small amount of glucose as glycogen. The average person carries 80,000–100,000 calories of stored fat but only 1,600–2,000 calories of glycogen. Evolutionarily, fat was the primary fuel for extended activity — glucose was reserved for acute, high-intensity demands.
3. What stops fat burning?
The primary inhibitor of fat burning is elevated insulin. Insulin activates fat storage pathways and directly suppresses the enzyme responsible for releasing stored fat. A diet high in refined carbohydrates and sugar keeps insulin chronically elevated, which keeps the body locked in fat-storage mode regardless of caloric intake. Even small insulin elevations are sufficient to halt lipolysis.
4. How do you switch your metabolism to fat burning?
The most direct way to shift from sugar-burning to fat-burning is to reduce dietary carbohydrates, particularly refined carbohydrates and sugar, which are the primary drivers of insulin elevation. Extending the daily fasting window also lowers insulin and allows the body to deplete glycogen stores before shifting to fat oxidation. Resistance exercise improves insulin sensitivity, making the transition more efficient. Metabolic flexibility — the ability to switch between fuel sources — improves as insulin sensitivity improves.
5. How long does it take to become fat-adapted?
Most people begin shifting toward fat oxidation within 1–2 weeks of consistent carbohydrate reduction. Full fat adaptation — where the body efficiently uses fat as its primary fuel at rest and during moderate activity — typically takes 4–8 weeks. During adaptation, some people experience temporary fatigue or brain fog as the metabolism adjusts. This phase resolves as mitochondrial fat-oxidation capacity increases.
6. Does exercise burn fat?
Yes, but the hormonal environment determines whether exercise is burning fat or sugar. Low-intensity aerobic exercise (Zone 2) burns primarily fat. High-intensity exercise burns primarily glucose. However, exercise also improves insulin sensitivity, which lowers baseline insulin levels over time and creates a better hormonal environment for fat burning throughout the day — including at rest.
Sources
Volek JS & Phinney SD — "The Art and Science of Low Carbohydrate Performance" (Beyond Obesity, 2012)
Cahill GF — "Fuel Metabolism in Starvation" (Annual Review of Nutrition, 2006) — https://pubmed.ncbi.nlm.nih.gov/16848698/
Paoli A et al. — "Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets" (European J Clinical Nutrition, 2013) — https://pubmed.ncbi.nlm.nih.gov/23801097/
Westman EC et al. — "Low-carbohydrate nutrition and metabolism" (Am J Clin Nutr, 2007) — https://pubmed.ncbi.nlm.nih.gov/17684196/
Hall KD et al. — "Energy expenditure and body composition changes after an isocaloric ketogenic diet" (Am J Clin Nutr, 2016) — https://pubmed.ncbi.nlm.nih.gov/27385608/
Lustig RH — "Fructose: It's Alcohol Without the Buzz" (Advances in Nutrition, 2013) — https://pubmed.ncbi.nlm.nih.gov/23408191/

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
