Edition: Hormones & Metabolism
18 March, 2026
In The News
Vol 1, Edition 15
What Is Ghrelin — The Hunger Hormone That Controls Your Appetite
Ghrelin is the hormone your stomach sends to your brain when it wants you to eat. Understanding how ghrelin works, why it spikes after dieting, and how to reduce ghrelin naturally through sleep, protein, and meal timing gives you a biological tool for managing hunger — rather than fighting it with willpower alone.
Published By: MAP30 Challenge
Authored By: John Shaw
Key Facts About Ghrelin: The 'Hunger Hormone'
28%
Rise in ghrelin after one night of poor sleep
Spiegel et al., PLOS Medicine 2004
~20 min
Delay before ghrelin drops after eating
Why eating slowly changes everthing
12-18 mo
Ghrelin stays elevated after weight loss
Sumithran et al., NEJM 2011
1999
Year ghrelin was discovered
Kojima et at., Nature
A persistent and damaging claim is that weight regain after dieting is a failure of discipline — that people who lose weight and gain it back simply lacked the willpower to maintain their habits. The hormonal evidence tells a completely different story. Research published in the New England Journal of Medicine found that ghrelin — the hormone that drives hunger — remained measurably elevated for a full 12 months after a calorie-restricted diet ended, creating a biological pressure toward weight regain that operates entirely independent of motivation or effort.
Imagine This. It is 10:30 in the morning. You had breakfast two hours ago. By any reasonable measure, you should not be hungry. And yet there it is — a pull toward food that feels less like preference and more like instruction. Not a craving exactly. Something more insistent than that.
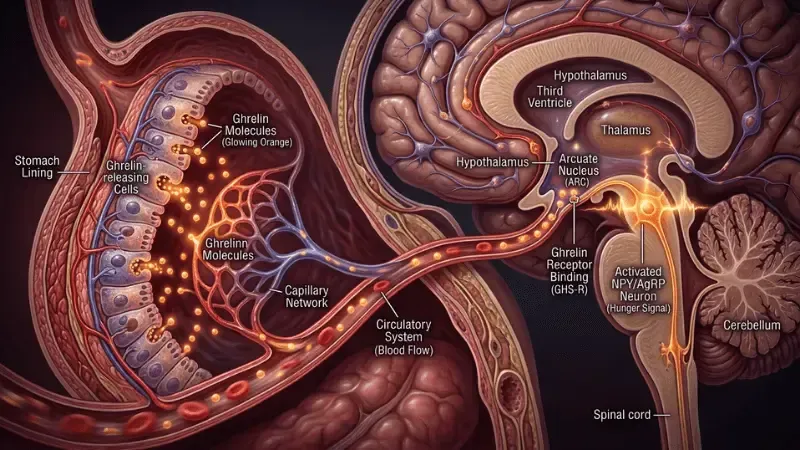
That signal has a name and a source. It is called ghrelin — a hormone produced primarily in your stomach that travels through the bloodstream to the hypothalamus in your brain and delivers one clear message: it is time to eat. Understanding what ghrelin is, how the ghrelin hormone works, and what drives it up or brings it down transforms hunger from something that happens to you into something you can actually influence.
Because ghrelin is not random. It runs on a biological logic — and once you understand that logic, you can work with it rather than against it.
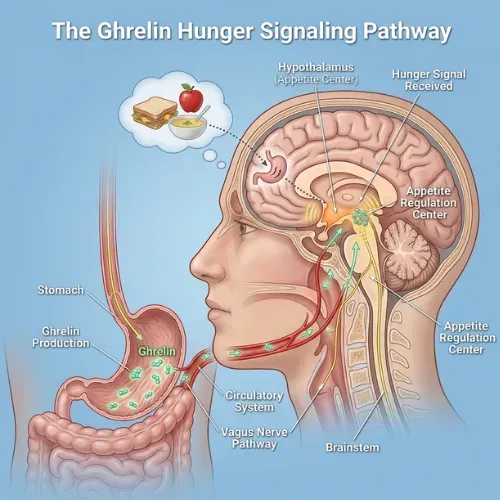
What Is Ghrelin and How Does the Ghrelin Hormone Work?
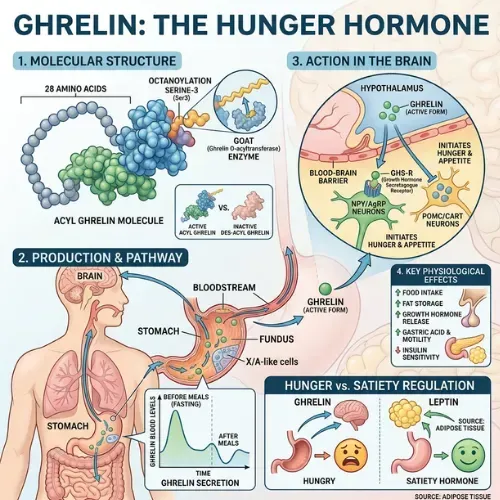
Ghrelin is a peptide hormone produced primarily by specialized cells lining the stomach, with smaller amounts produced in the duodenum, pancreas, and brain. It was identified in 1999 by Masayasu Kojima and colleagues at the National Cardiovascular Center Research Institute in Japan — and quickly recognized as the only known circulating hormone that actively stimulates appetite rather than suppressing it.
Here is how the ghrelin hormone works: when your stomach is empty and energy intake has been low, ghrelin is released into the bloodstream. It travels to the hypothalamus — the brain's control center for hunger, metabolism, and energy balance — and activates receptors that generate the subjective experience of hunger. At the same time, ghrelin signals the pituitary gland to release growth hormone and activates the brain's reward centers, making food feel more appealing and the drive to seek it more urgent.
Ghrelin levels follow a predictable daily rhythm. They rise before anticipated mealtimes, peak just before eating, and drop within about twenty minutes of food intake — which is one biological reason eating slowly and pausing before taking more food is genuinely effective. Between meals, ghrelin rises again in a cyclical pattern tied to meal frequency and timing.
“Ghrelin is the only known hormone that actively drives you to eat. Every other appetite hormone — leptin, insulin, GLP-1, CCK — works by suppressing hunger. Ghrelin is the one pushing the accelerator.”
Leptin and Ghrelin: The Two Sides of Hunger
To understand ghrelin fully, you need its counterpart. Ghrelin and leptin are the two primary hormones regulating hunger and energy balance — and they work in direct opposition.
Leptin is produced by fat cells and signals the brain that long-term energy reserves are sufficient: reduce appetite, allow fat burning. Ghrelin is produced by the stomach and signals the brain that short-term energy is needed: increase appetite, seek food. In a healthy metabolism, these signals are balanced — leptin keeps ghrelin in check between meals, and ghrelin rises appropriately before meals to drive eating.
When this balance breaks down — through poor sleep, chronic stress, insulin resistance, or years of dieting — ghrelin can become chronically elevated while leptin signaling simultaneously degrades. The result is a body that is simultaneously receiving a constant drive-to-eat signal and failing to receive the adequate-energy signal that would offset it. Hunger becomes relentless not because of weakness, but because both sides of the hormonal equation are working against the person trying to manage their weight.
| Ghrelin — The Hunger Signal | Leptin — The Fullness Signal |
|---|---|
| Produced in the stomach | Produced in fat cells |
| Signals the brain: time to eat | Signals the brain: energy reserves adequate |
| Rises before meals, drops after eating | Rises as fat stores increase, drops as they fall |
| Short-term hunger trigger | Long-term energy reserve communicator |
| Rises sharply with sleep deprivation | Falls with sleep deprivation |
| Stays elevated 12–18 months after weight loss | Drops sharply after calorie restriction |
| Stimulated by cortisol and chronic stress | Disrupted by chronic insulin elevation |
Why Dieting Makes Ghrelin Worse — The Clinical Evidence
This is the mechanism behind the most frustrating weight loss experience: doing everything right, losing the weight — and then watching it return despite your best efforts to hold the line on hunger.
When you restrict calories significantly, ghrelin rises. This is your body's predictable response to a perceived energy deficit: produce more of the hormone that drives eating. The more aggressive the restriction, the more ghrelin climbs. And crucially, it does not return to baseline once the diet ends.
🔬 CLINICAL STUDY
Sumithran P et al. — New England Journal of Medicine, 2011
Researchers followed 50 overweight adults through a 10-week very-low-calorie diet, then monitored them for 12 months. At the one-year mark, participants had regained a significant portion of lost weight — and their ghrelin levels remained measurably higher than pre-diet baselines. The study also found that appetite-suppressing hormones including leptin, peptide YY, and GLP-1 remained persistently lower than baseline a full year after the diet ended. The authors concluded that weight loss triggers long-lasting hormonal changes that favor regain — and that these changes persist well beyond the period of active restriction.
This is not a minor finding. It means that the hunger you feel six months or a year after losing weight is not a discipline failure — it is a documented hormonal state. Your body is still producing elevated ghrelin levels it generated during the diet, still driving you toward the calorie intake it considers normal. The biology of weight regain is not a character flaw. It is a measurable, predictable, hormonal event.
This is also why approaches that only address calories — without addressing the hormonal environment driving hunger — produce results that are real but rarely permanent.
WHAT DRIVES GHRELIN UP
Calorie restriction and skipping meals
Poor sleep — even one night raises ghrelin ~28%
Chronic stress and elevated cortisol
Rapid weight loss
Low protein intake
Eating quickly — ghrelin takes ~20 minutes to fall after food intake
Irregular meal timing — the body anticipates meals and spikes ghrelin in advance
Controlling Ghrelin Through Sleep — What the Research Shows
Sleep is the single most powerful and most underused tool for ghrelin regulation. The evidence is not subtle.
Research participants who were sleep-restricted consumed on average 300 to 500 additional calories per day compared to well-rested conditions — driven by ghrelin elevation and the dopamine-reward system activation that ghrelin triggers in the brain. Chronic partial sleep restriction, which describes the sleep patterns of a significant portion of working adults, produces a persistent ghrelin elevation that dietary changes alone struggle to compensate for.
The implication is direct: if you are trying to manage hunger and lose weight while consistently sleeping five to six hours a night, you are fighting a hormonal disadvantage that has nothing to do with food choices. Sleep is not optional for ghrelin control. It is foundational to it.
SLEEP AND GHRELIN: THE RESEARCH NUMBERS
4–5 hours of sleep raises ghrelin ~28% the following day
The same restriction reduces leptin ~18%
Sleep-deprived individuals consume 300–500 more calories per day on average
The drive is specifically toward high-carb, high-calorie foods
Chronic partial sleep restriction produces persistent hormonal disruption
7–9 hours is the research-supported target for ghrelin regulation
“The hunger you feel after a diet isn't a sign you've failed. It's ghrelin — still elevated, still doing exactly what biology programmed it to do. The fight is not with your willpower. It's with your hormones.”
How to Reduce Ghrelin Naturally
Ghrelin cannot be eliminated — and should not be. Its pre-meal rise is part of healthy digestive preparation. The goal is to prevent the chronic, sustained elevation that makes hunger unmanageable and weight maintenance so difficult. Here are the interventions with the strongest evidence.
1
Prioritize Sleep — Seven to Nine Hours
This is the most direct lever for ghrelin control available. Addressing sleep before optimizing diet is not backwards — it is strategic. A sleep-deprived person starts every day with a 28% ghrelin disadvantage. No dietary change fully compensates for that. Seven to nine hours of quality sleep is not a lifestyle luxury. It is a hormonal requirement.
2
Eat Adequate Protein at Every Meal
Protein is the most ghrelin-suppressive macronutrient. High-protein meals produce a greater and more sustained drop in ghrelin compared to equivalent-calorie meals high in carbohydrates or fat. Studies consistently show that increasing protein to 25–30% of caloric intake reduces ghrelin, extends satiety between meals, and reduces total daily calorie intake without deliberate restriction. Eggs, meat, fish, and dairy are the most effective protein sources for ghrelin suppression.
3
Eat Slowly — Give Ghrelin Time to Drop
Ghrelin takes approximately twenty minutes to fall after food intake begins. Eating quickly means consuming significantly more food than needed before the hormonal off-signal registers. Slowing down — chewing thoroughly, putting the fork down between bites, removing screen distractions — is advice grounded in biology, not etiquette. It gives ghrelin time to drop before hunger overrides portion awareness.
4
Maintain Consistent Meal Timing
Ghrelin operates on a learned anticipatory rhythm — it rises before expected mealtimes, which is why hunger often arrives on schedule regardless of actual energy needs. Consistent meal timing trains ghrelin to rise and fall predictably rather than spiking erratically throughout the day. Skipping meals or eating at highly variable times produces larger, more disruptive ghrelin spikes and makes hunger harder to manage over the course of the day.
5
Manage Chronic Stress
Cortisol directly stimulates ghrelin secretion. Chronic psychological stress produces sustained cortisol elevation, which keeps ghrelin elevated and drives a persistent biological pull toward high-calorie, high-carbohydrate food. This is the hormonal mechanism behind stress eating — not emotional weakness, but cortisol driving ghrelin, driving appetite. For many people, stress management is as important to ghrelin control as any dietary change.
6
Reduce Ultra-Processed Foods and Refined Carbohydrates
Meals high in refined carbohydrates and ultra-processed foods produce a rapid post-meal ghrelin drop followed by a sharp rebound as blood sugar falls. Whole food meals — particularly those high in protein and fiber — produce a slower, more sustained ghrelin suppression. Over time, a diet built around whole foods stabilizes ghrelin patterns. A diet built around processed carbohydrates recreates the spike-and-crash hunger cycle that makes overeating nearly inevitable.
Ghrelin, Leptin, and the Metabolic Picture

Ghrelin does not operate in isolation. It is one signal in a hormonal system that includes leptin, insulin, cortisol, and a network of other hormones all communicating simultaneously about energy reserves, stress, sleep, and food quality.
What the Sumithran NEJM study, the Spiegel sleep study, and decades of metabolic research collectively establish is this: hunger is not primarily a matter of discipline. It is a hormonally regulated biological state that can be running at maximum intensity for physiological reasons completely outside a person's conscious control. The person who can't stop eating after a diet is not weak. They are experiencing a documented, measurable, hormonal event.
The practical implication is that managing hunger requires managing the hormonal system that produces it. That means addressing sleep as a non-negotiable foundation, reducing the dietary patterns that keep ghrelin chronically elevated, eating adequate protein to give ghrelin's suppressive signals the best raw material to work with, and giving the body time between meals to let the system regulate itself.
This is what working with your biology rather than against it actually looks like. Not starvation. Not willpower. A hormonal environment that makes eating less feel natural rather than heroic.
“Hunger is not a character flaw. It is a hormone. And like every hormone, it responds to the conditions you create.”
Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Individual metabolic responses vary. Consult a qualified healthcare provider before making significant changes to your diet or lifestyle.
References
Kojima M et al. — "Ghrelin is a growth-hormone-releasing acylated peptide from stomach" (Nature, 1999) — https://pubmed.ncbi.nlm.nih.gov/10604470/
Sumithran P et al. — "Long-term persistence of hormonal adaptations to weight loss" (New England Journal of Medicine, 2011) — https://pubmed.ncbi.nlm.nih.gov/22082085/
Spiegel K et al. — "Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite" (PLOS Medicine, 2004) — https://pubmed.ncbi.nlm.nih.gov/15602591/
Cummings DE et al. — "A preprandial rise in plasma ghrelin levels suggests a role in meal initiation in humans" (Diabetes, 2001) — https://pubmed.ncbi.nlm.nih.gov/11473029/
Leidy HJ et al. — "The role of protein in weight loss and maintenance" (American Journal of Clinical Nutrition, 2015) — https://pubmed.ncbi.nlm.nih.gov/25926512/
Wren AM et al. — "Ghrelin enhances appetite and increases food intake in humans" (Journal of Clinical Endocrinology & Metabolism, 2001) — https://pubmed.ncbi.nlm.nih.gov/11739433/
This article is part of our Hormones & Metabolism series. Hormones & Metabolism
Latest Articles

Insulin Resistance
You don't need a diabetes diagnosis to have insulin resistance. Millions of Americans are living with it right now — tired, foggy...

Calorie Deficit Diet?
The calorie deficit model has been the foundation of weight loss advice for over a century. But millions of people follow it precisely...

The Food Pyramid
For three decades, Americans were told to eat 6 to 11 servings of grains per day and avoid fat at all costs. The science behind that advice was always...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
FAQ's
1. What is ghrelin?
Ghrelin is a peptide hormone produced primarily in the stomach that signals hunger to the brain. It is often called the hunger hormone because its primary function is to stimulate appetite before meals and promote food-seeking behavior. Ghrelin rises in the hours before eating and falls after a meal. It also stimulates the release of growth hormone and plays a role in energy balance, fat storage, and metabolic rate regulation.
2. Why does dieting increase ghrelin?
Caloric restriction consistently elevates ghrelin levels as a biological defense against starvation. When the body detects reduced energy intake and falling fat stores, ghrelin rises to drive hunger and motivate food-seeking behavior. Research by Cummings et al. (2002) found that ghrelin levels were significantly higher in subjects who had lost weight through caloric restriction compared to never-obese controls — and remained elevated for months after weight loss, explaining why hunger persists long after a diet ends.
3. How does ghrelin cause weight regain after dieting?
Ghrelin drives weight regain through two mechanisms. First, chronically elevated ghrelin after weight loss produces persistent hunger that erodes dietary adherence over time. Second, elevated ghrelin promotes fat storage and reduces energy expenditure — the metabolism adapts to what it perceives as a starvation state. This is the biological basis of the 95% weight regain rate: the body is actively fighting to restore lost fat through hormonal mechanisms that operate independently of willpower.
4. Does intermittent fasting lower ghrelin?
Yes — and this is a key advantage of intermittent fasting over continuous caloric restriction. Intermittent fasting adapts the ghrelin rhythm rather than chronically elevating it. Research shows that after an adaptation period of 1–2 weeks, ghrelin pulses align with the eating window rather than spiking continuously. This means hunger becomes predictable and manageable rather than constant. The same caloric reduction that elevates ghrelin when spread throughout the day produces smaller ghrelin responses when compressed into a fasting protocol.
5. What is the connection between ghrelin and sleep?
Sleep is one of the primary regulators of ghrelin. Sleep deprivation consistently elevates ghrelin and suppresses leptin simultaneously — a double hormonal hit that increases hunger and reduces satiety. Research by Spiegel et al. (2004) found that two nights of sleep restriction (4 hours) elevated ghrelin by 28% and reduced leptin by 18%, producing a significant increase in appetite and preference for high-calorie foods. Poor sleep is one of the most reliable ways to dysregulate hunger hormones.
6. How do you reduce ghrelin levels?
Ghrelin is best managed through: consistent sleep of 7–9 hours (sleep deprivation is one of the strongest ghrelin elevators); dietary protein at meals (protein suppresses ghrelin more effectively than carbohydrates or fat); intermittent fasting protocols that adapt the ghrelin rhythm rather than chronically suppress appetite; and visceral fat reduction, which improves the overall hormonal environment. Chronic caloric restriction is the least effective ghrelin management strategy because it elevates baseline ghrelin continuously.
Sources
Cummings DE et al. — "Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery" (NEJM, 2002)
https://pubmed.ncbi.nlm.nih.gov/12120942/
Spiegel K et al. — "Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels" (Annals of Internal Medicine, 2004)
https://pubmed.ncbi.nlm.nih.gov/15583226/
Rosenbaum M et al. — "Long-term persistence of adaptive thermogenesis in subjects who have maintained a reduced body weight" (AJCN, 2008)
https://pubmed.ncbi.nlm.nih.gov/18842775/
Tschop M et al. — "Ghrelin induces adiposity in rodents" (Nature, 2000)
https://pubmed.ncbi.nlm.nih.gov/10935631/
Wren AM et al. — "Ghrelin enhances appetite and increases food intake in humans" (Journal of Clinical Endocrinology & Metabolism, 2001)

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
