Edition: Hormones & Metabolism
18 March, 2026
In The News
Vol 1, Edition 14
How Leptin Works — and Why Your Brain Thinks You're Starving
Leptin is the hormone your fat cells use to tell your brain you have enough stored energy. When it works, hunger is manageable and weight regulates itself. When leptin resistance sets in, your brain thinks you're starving — even when you're not. Understanding what causes leptin resistance, and how to fix it, changes everything about why diets fail.

Published By: MAP30 Challenge
Authored By: John Shaw
You have tried eating less. You have tried moving more. You have white-knuckled your way through calorie deficits that left you exhausted, irritable, and thinking about food every waking hour. And then, at some point, you gave in — not because you lacked willpower, but because your brain was issuing a biological alarm so loud it was impossible to ignore.
That alarm has a name. It's called leptin resistance — and it is one of the most underdiagnosed drivers of chronic hunger, failed dieting, and stubborn weight gain. Understanding how leptin works in the body, what causes leptin resistance, and how to fix it reframes the entire weight loss conversation from a discipline problem into a hormonal one.
Because that's what it is.
What Is Leptin and How Does It Work?
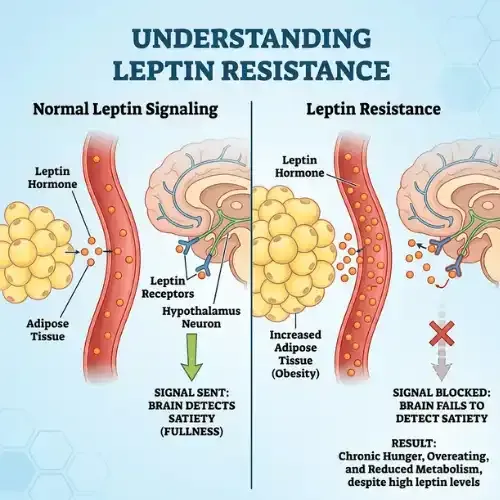
Leptin is a hormone produced by your fat cells — specifically by adipose tissue. Its primary job is to act as a long-range signal between your body's energy reserves and your brain. When fat stores are adequate, fat cells release leptin into the bloodstream. Leptin travels to the hypothalamus — the region of the brain that regulates hunger, metabolism, and energy balance — and delivers a clear message: we have sufficient stored energy. Reduce appetite. Allow fat burning to continue.
In a healthy metabolic state, this system is self-regulating and elegant. As fat stores increase, leptin rises, appetite decreases, and the body naturally limits further fat accumulation. As fat stores decrease, leptin falls, appetite increases, and the body drives you back toward eating. The system is designed to keep energy balance stable over the long term without conscious effort.
Think of leptin as the fuel gauge on a car. When the tank is full, the gauge reads full and you don't think about stopping for gas. When it drops, the gauge signals low and you respond. Leptin is that gauge — communicating the state of your long-term energy reserves directly to the control center that manages hunger and metabolism.
Leptin doesn't just regulate hunger. It tells your brain whether it's safe to burn stored fat — or whether survival mode needs to kick in.”
What Is Leptin Resistance — and What Causes It?
Leptin resistance is what happens when the brain stops responding normally to leptin's signal. The hormone is still being produced — often in large quantities. The fat cells are still releasing it. But the hypothalamus has become desensitized to it, like a smoke detector with a dead battery. The alarm is going off but nothing responds.
The result is that the brain, receiving no clear leptin signal, concludes that the body is in an energy-deficient state — even when fat stores are full. It responds exactly as it would to actual starvation: it increases hunger, reduces the drive to move, slows metabolism, and does everything in its power to drive calorie intake up and energy expenditure down.
This is not a character flaw. This is your brain executing its most fundamental survival program — and executing it effectively — based on faulty information.
WHAT CAUSES LEPTIN RESISTANCE?
• Chronic elevation of insulin — the single most significant driver
• Chronic inflammation — particularly in the hypothalamus itself
• Ultra-processed food consumption — especially high fructose intake
• Sleep deprivation — even one night reduces leptin by up to 18%
• Chronic stress — cortisol disrupts leptin signaling pathways
• Excess body fat — creates a self-reinforcing cycle of resistance
The cruel irony of leptin resistance is that it is self-reinforcing. The more fat you carry, the more leptin your fat cells produce. The more leptin flooding the system, the more desensitized the brain becomes to the signal. The more desensitized the brain, the more it drives hunger and fat storage. The more fat you accumulate, the more leptin you produce. The cycle continues.
This is why people with obesity often have leptin levels three to four times higher than lean individuals — and yet their brains are responding as if they have almost none.
~65%
of people with obesity show leptin resistance
Friedman JM, Nature Medicine 2019
3–4×
higher leptin in obese vs. lean individuals
yet the brain stops responding
24 hrs
sleep deprivation drops leptin by ~18%
Spiegel et al., PLOS Medicine 2004
Years
leptin resistance can develop silently
before weight gain becomes visible
How Insulin and Leptin Work Together — and Against You
Leptin and insulin are the two most important hormones in the regulation of body weight and energy balance. They work in tandem — and when one is disrupted, the other almost always follows.
Insulin is the short-term fuel-management signal. After a meal, insulin rises to manage blood glucose, drive nutrients into cells, and signal fat storage. Leptin is the long-term energy-reserve signal, communicating the state of fat stores over days and weeks. In a healthy metabolism, these two systems are coordinated: insulin rises and falls with meals, leptin rises and falls with fat stores, and the brain receives accurate information from both.
When insulin becomes chronically elevated — through a diet high in refined carbohydrates and processed foods — it begins to interfere directly with leptin signaling. Chronically high insulin promotes fat storage, which increases leptin production. But high insulin also promotes inflammation in the hypothalamus, degrading the very receptors that leptin needs to deliver its message. The result is that insulin resistance and leptin resistance tend to develop together, compound each other, and create a metabolic environment in which the body is simultaneously storing fat and behaving as if it's starving.
“Insulin resistance and leptin resistance are not separate problems. They are two expressions of the same underlying metabolic dysfunction — and they feed each other.”
THE INSULIN-LEPTIN VICIOUS CYCLE
1. High-carb diet → chronic insulin elevation
2. Chronic insulin → increased fat storage
3. More fat → more leptin produced
4. Chronic high leptin → hypothalamus becomes desensitized
5. Brain thinks it's starving → hunger increases, metabolism slows
6. More eating → more fat storage → cycle continues
Why Diets Don't Work When Leptin Resistance Is Present
This is the mechanism behind the most frustrating experience in weight loss: doing everything right and getting nowhere.
When leptin resistance is established, calorie restriction makes it worse. Cut calories significantly and leptin levels drop sharply — because falling fat stores reduce leptin production. The already-resistant brain, now receiving even less leptin signal, escalates its starvation response. Hunger intensifies. Metabolism slows further. The drive to eat becomes physiologically overwhelming.
Studies following people who have lost significant weight through calorie restriction consistently show the same pattern: leptin drops far more than would be expected from fat loss alone, hunger hormones rise, and the metabolic rate suppresses. The body is actively working to restore its previous fat stores. This is not weakness. This is biology doing exactly what it was designed to do.
The problem is not that people can't follow diets. The problem is that conventional dieting — eat less, move more — directly activates the hormonal machinery designed to make weight loss fail. Until leptin sensitivity is restored, sustainable weight loss is working against the most powerful survival systems in the human body.

SIGNS YOU MAY HAVE LEPTIN RESISTANCE
• Hunger that returns quickly after meals — even large ones
• Strong cravings, especially for carbohydrates and sugar
• Difficulty losing weight despite calorie restriction
• Fatigue, especially in the afternoon
• Difficulty feeling satisfied — fullness signals are delayed or absent
• Weight that plateaus quickly on a diet and rebounds rapidly afterward
• Poor sleep or sleep that doesn't feel restorative
How to Fix Leptin Resistance
Leptin sensitivity cannot be restored by taking a supplement. There is no leptin pill, patch, or injection that reliably works for weight loss in humans — leptin administered externally does not solve the resistance problem any more than shouting louder fixes a deaf phone. The solution is to reduce the conditions that created the resistance in the first place.
The most effective interventions target insulin first — because chronically elevated insulin is the primary driver of the hypothalamic inflammation that causes leptin resistance. Lower insulin, and you begin to lower the inflammation that is blocking the leptin signal. The sequence matters.
1
Reduce Refined Carbohydrates and Added Sugar
The most direct lever for lowering chronic insulin elevation is reducing the foods that drive it: processed foods, refined grains, added sugars, and sweetened beverages. This doesn't require a strict ketogenic diet — meaningful reduction is sufficient to begin lowering insulin and reducing hypothalamic inflammation. As insulin drops, the conditions that drive leptin resistance begin to resolve.
2
Prioritize Sleep
Sleep is one of the most powerful and most underutilized tools for leptin regulation. A single night of sleep deprivation reduces leptin by approximately 18% and raises ghrelin (the hunger hormone) by 28%. Chronic sleep restriction produces persistent hormonal disruption that dietary changes alone cannot fully compensate for. Seven to nine hours of quality sleep is not optional for leptin recovery — it is a biological requirement.
3
Eat in a Way That Lowers Inflammation
Hypothalamic inflammation is the mechanism by which leptin resistance develops and is maintained. Reducing dietary sources of inflammation — ultra-processed foods, seed oils high in omega-6 fatty acids, added sugars, and refined grains — while increasing anti-inflammatory whole foods creates the conditions for leptin receptor sensitivity to recover. This is a slow process measured in weeks, not days.
4
Allow Time Between Meals
Constant eating keeps insulin elevated and prevents leptin signaling from functioning properly. Allowing three to five hours between meals — without snacking — gives insulin time to fall and leptin's long-term signaling to operate without interference. As fat burning improves and insulin sensitivity is restored, the time between meals when hunger is manageable naturally extends. This is what metabolic health feels like in practice.
5
Manage Stress
Cortisol, the primary stress hormone, directly impairs leptin sensitivity and promotes fat storage — particularly visceral fat, which is itself a driver of inflammation and leptin resistance. Chronic psychological stress creates a sustained cortisol elevation that undermines dietary and sleep improvements. Stress management is not peripheral to metabolic recovery. For many people, it is central to it.
The Bigger Picture: Leptin, Insulin, and Metabolic Recovery

Leptin resistance doesn't exist in isolation. It develops alongside insulin resistance, is worsened by the same dietary patterns that drive insulin resistance, and resolves through the same interventions that restore insulin sensitivity. The two conditions share a common cause and a common solution.
This is why approaches that focus only on calories miss the point. Hunger is not simply a matter of discipline — it is a hormonally regulated signal that can be running at maximum intensity for biological reasons completely outside a person's conscious control. When leptin resistance is present, the experience of hunger is not exaggerated or imaginary. It is real, it is physiologically driven, and it will not respond to willpower indefinitely.
Restoring leptin sensitivity — by reducing insulin, improving sleep, lowering inflammation, and giving the body time between meals — doesn't just make weight loss easier. It makes hunger manageable. It makes the biology work with you instead of against you. And that is the difference between a diet you can sustain and one you can't.
“You are not hungry because you lack discipline. You are hungry because your brain is not receiving the signal that your fat cells are full. Fix the signal — and the hunger changes.”
⚠️ Medical Disclaimer:
This article is for educational purposes only and does not constitute medical advice. Individual metabolic responses vary. Consult a qualified healthcare provider before making significant changes to your diet or lifestyle, especially if you have a diagnosed metabolic condition.
This article is part of our Hormones & Metabolism series. Hormones & Metabolism
Latest Articles

Intermittent Fasting
Most people think fasting is about willpower. The biology tells a different story. When you stop eating, your body doesn't go into starvation mode — it goes into repair mode...
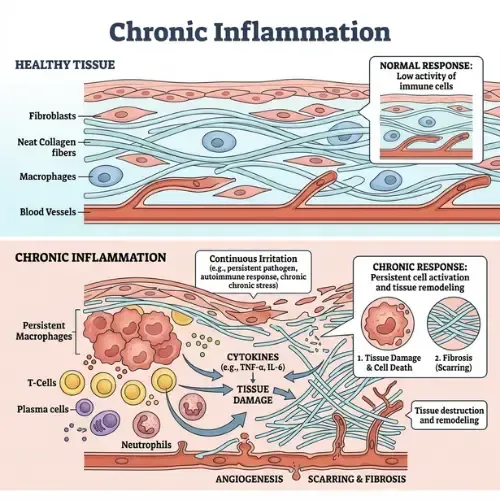
Chronic Inflammation
Chronic inflammation is not the redness and swelling of an injury. It is a silent, systemic biological state that disrupts hormones, impairs insulin signaling, and drives fat storage...
How Does Mitochondria Work
Persistent fatigue, mid-morning crashes, brain fog, and poor sleep are not personality traits or signs of aging. They are symptoms — and for a large portion of the population...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
Disclaimer: The information in this article is for educational purposes only and does not constitute medical advice. Fatigue and related symptoms can have many causes, some of which require medical evaluation and treatment. Nothing in this article should be interpreted as a recommendation to change, stop, or start any medication or treatment plan. Always consult a qualified healthcare provider before making significant changes to your diet or lifestyle..
FAQ's
1. What is leptin?
Leptin is a hormone produced by fat cells (adipocytes) that signals the brain — specifically the hypothalamus — about the body’s energy stores. When fat stores are adequate, leptin rises, suppressing hunger and increasing energy expenditure. When fat stores drop, leptin falls, triggering hunger and reducing metabolic rate. Leptin is often called the satiety hormone because its primary function is to tell the brain that the body has enough stored energy and does not need to eat.
2. What is leptin resistance?
Leptin resistance is a condition in which the brain stops responding normally to leptin’s signal despite adequate or elevated leptin levels. In leptin resistance, fat cells produce plenty of leptin but the hypothalamus cannot receive the signal effectively — so the brain acts as if the body is starving, driving hunger, slowing metabolism, and promoting fat storage. Leptin resistance is found in the majority of obese individuals, which is why hunger persists even when fat stores are abundant.
3. What causes leptin resistance?
The primary drivers of leptin resistance are chronic inflammation, elevated triglycerides (which physically block leptin from crossing the blood-brain barrier), sleep deprivation, and chronically elevated insulin. High-fructose diets are particularly damaging because fructose metabolism elevates triglycerides and promotes the liver fat accumulation that drives systemic inflammation. The result is a self-reinforcing cycle: obesity drives leptin resistance, and leptin resistance drives further fat storage.
4. How does leptin affect weight loss?
Leptin resistance explains why calorie restriction consistently fails long-term. When calories are reduced and fat stores decrease, leptin falls. The brain interprets this as starvation and responds by increasing hunger, reducing energy expenditure, and promoting fat storage at the first opportunity. This is the biological mechanism behind the 95% weight regain rate after caloric restriction diets. Restoring leptin sensitivity — rather than fighting a leptin-resistant brain with willpower — is the key to sustainable fat loss.
5. How do you fix leptin resistance?
Leptin resistance improves with interventions that reduce inflammation and triglycerides: carbohydrate restriction (particularly eliminating fructose and refined carbohydrates), quality sleep (leptin is regulated by circadian rhythm and peaks during deep sleep), intermittent fasting, and visceral fat reduction. Exercise, particularly resistance training, also improves leptin sensitivity. There is no supplement that directly restores leptin sensitivity — the intervention is dietary and lifestyle-based.
6. Is leptin resistance the same as insulin resistance?
They are distinct but closely related. Both involve cells becoming unresponsive to a hormonal signal. Both are driven by similar dietary and lifestyle factors. And critically, elevated insulin promotes leptin resistance, and leptin resistance worsens insulin signaling. They tend to develop together and are both features of metabolic syndrome. Addressing insulin resistance through carbohydrate reduction typically improves leptin sensitivity simultaneously, which is why low-carbohydrate diets produce improvements in both hunger regulation and fat burning.
Sources
Friedman JM — "Obesity in the new millennium" (Nature, 2000)
https://pubmed.ncbi.nlm.nih.gov/10766249/
Halaas JL et al. — "Weight-reducing effects of the plasma protein encoded by the obese gene" (Science, 1995)
https://pubmed.ncbi.nlm.nih.gov/7624777/
Banks WA et al. — "Triglycerides induce leptin resistance at the blood-brain barrier" (Diabetes, 2004)
https://pubmed.ncbi.nlm.nih.gov/14747278/
Myers MG et al. — "Mechanisms of leptin action and leptin resistance" (Annual Review of Physiology, 2008)
https://pubmed.ncbi.nlm.nih.gov/17937601/
Spiegel K et al. — "Sleep curtailment in healthy young men is associated with decreased leptin levels" (Annals of Internal Medicine, 2004)

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
