Edition: Gut, Inflammation & Recovery
11 March, 2026
In The News
Vol 1, Edition 7
How Mitochondria Produce Energy — and Why You’re Tired Every Morning
Persistent fatigue, mid-morning crashes, brain fog, and poor sleep are not personality traits or signs of aging. They are symptoms — and for a large portion of the population, they trace back to a single root cause: mitochondrial dysfunction driven by what we eat every day.
Edition: Gut, Inflammation & Recovery
12 March, 2026
In The News
Vol 1, Edition 6
How Does Mitochondria Work — And Why It Controls Your Energy, Fat Burning, and Metabolism
Persistent fatigue, mid-morning crashes, brain fog, and poor sleep are not personality traits or signs of aging. They are symptoms — and for a large portion of the population, they trace back to a single root cause: mitochondrial dysfunction driven by what we eat every day.
Published By: MAP30 Challenge
Authored By: John Shaw
~37T
estimated cells in the human body — each with its own mitochondrial power supply
Bianconi et al., Annals of Human Biology, 2013
20%
of total resting body energy consumed by the brain — its preferred fuel is ketones
PMC7699472 / Frontiers in Molecular Neuroscience
>50%
of daily caloric intake in Western diets comes from ultra-processed foods
ScienceDirect, 2025 UPF cardiovascular review
ATP
adenosine triphosphate — the cellular energy currency produced by every mitochondrion in your body
Basic biochemistry / NIH reference
Why You’re Tired Every Morning — and What It Says About Cellular Energy
The alarm goes off. You have slept seven or eight hours. You sit up slowly, wait for the fog to clear, and reach for your phone. By the time you have made it to the kitchen, you already need coffee. You eat breakfast. An hour later, you are crashing again.
For millions of people, this is not an occasional rough morning. It is every morning. And the explanation they are most often given — that they need better sleep, less stress, more exercise — is not wrong exactly, but it misses the mechanism underneath. The question is not just why you feel tired. It is why your body is failing to produce adequate energy in the first place.
The answer, increasingly supported by research, begins at the cellular level — with structures called mitochondria, and with the fuel you have been asking them to burn.
Understanding how mitochondria produce energy helps explain why some people wake up exhausted even after a full night of sleep.
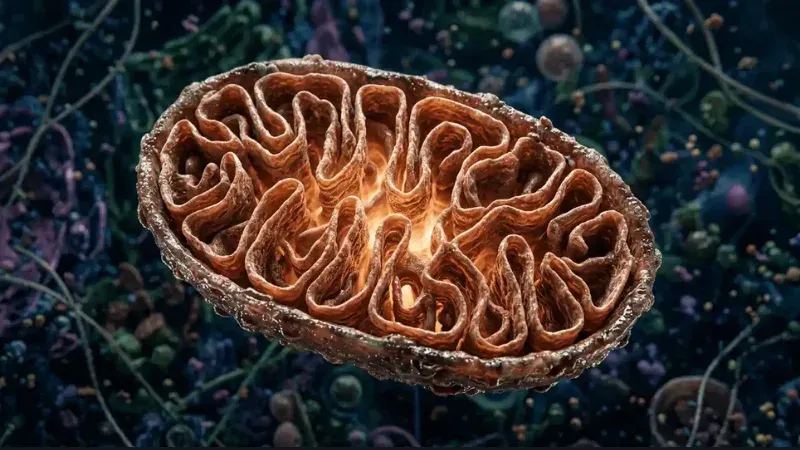
What Mitochondria Are and What They Actually Do
Mitochondria are the structures that turn nutrients into usable cellular energy. Every cell in the human body — with a few exceptions, such as mature red blood cells — contains mitochondria. The number varies significantly by cell type. Liver cells may contain between 1,000 and 2,000 mitochondria each. Cardiac muscle cells, which require continuous, uninterrupted energy output, may contain even more. Skeletal muscle cells are similarly dense. Across an estimated 37 trillion cells in the human body, the total mitochondrial count runs into the hundreds of trillions.
Their primary function is to produce adenosine triphosphate — ATP — the universal energy currency of cellular biology. Every physical movement, every thought, every heartbeat, every immune response requires ATP. When mitochondria are functioning well, ATP is produced efficiently and in sufficient quantity. When they are not, the shortfall is felt throughout the body as fatigue, cognitive impairment, and a pervasive sense of depletion that sleep alone does not resolve.
What makes mitochondria unusual among cellular structures is that they carry their own separate DNA — distinct from the nuclear DNA in the cell's nucleus. This is not incidental.

Mitochondria are believed to have originated as independent bacteria that were incorporated into early eukaryotic cells approximately 1.5 to 2 billion years ago — an evolutionary arrangement called endosymbiosis. Their separate genome is a remnant of that origin and makes them uniquely sensitive to environmental conditions, including the metabolic environment created by what we eat.
I
“Mitochondria are not simply passive structures inside your cells. They are dynamic, responsive, and — when the conditions driving their dysfunction are removed — capable of significant recovery.”
How Mitochondria Produce ATP From Glucose and Ketones
Mitochondria produce ATP from two primary fuel sources: glucose, derived from carbohydrates, and ketone bodies, derived from stored fat. ATP is the main energy currency of the body, and mitochondria generate it through oxidative phosphorylation. Understanding how these two fuels affect ATP production helps explain why energy, mental clarity, and metabolic health can feel very different depending on what the body is burning.
When you eat carbohydrates, they are broken down into glucose, which enters the bloodstream and triggers an insulin response. Glucose is then transported into cells, where it enters the mitochondria to undergo oxidative phosphorylation and produce ATP. This system works efficiently under normal circumstances. But it has a significant limitation: glucose metabolism produces more reactive oxygen species — ROS — than fat-based metabolism. ROS are chemically unstable molecules that, in excess, damage cellular structures, including the mitochondria themselves. This process is called oxidative stress.
Ketone bodies — primarily beta-hydroxybutyrate (BHB) and acetoacetate — are produced by the liver from fatty acids during periods of low carbohydrate intake, fasting, or extended exercise. They enter mitochondria through a different metabolic pathway, producing ATP more efficiently and generating substantially fewer reactive oxygen species per unit of energy produced. The result is less oxidative stress, less mitochondrial damage, and a cleaner energy cycle.
The brain is particularly relevant here. The brain accounts for approximately 20% of the body's total resting energy expenditure despite representing only about 2% of body weight. It runs continuously — including during sleep — and its energy demands do not switch off. Research published in journals including Frontiers in Molecular Neuroscience and the Journal of Neuropsychiatry and Clinical Neurosciences has documented that when both glucose and ketones are available, the brain preferentially uses ketones. PET imaging studies in humans have shown that ketone uptake by the brain increases in direct proportion to blood ketone concentration, independent of glucose availability — a pattern described as a "push" mechanism, in contrast to glucose which is "pulled" based on demand.
This has a practical implication for morning fatigue that is rarely discussed. While you sleep, your brain continues consuming energy. What it burns during those hours — and how efficiently it burns it — affects whether you wake feeling rested or depleted. A brain running on glucose from a high-carbohydrate diet the night before is burning a fuel that produces more oxidative byproducts per unit of ATP. A brain adapted to using ketones is burning a cleaner fuel through a more efficient pathway. The quality of the fuel matters, not just the quantity.
Fuel Source
Key Metabolic Characteristics
Glucose (from dietary carbohydrates)
Requires insulin for cellular uptake; higher ROS production per unit of ATP; can cause blood sugar spikes and subsequent crashes; requires insulin to cross the blood-brain barrier via GLUT transporters
Ketone bodies (from stored fat)
Do not require insulin to cross the blood-brain barrier; lower ROS production; more ATP generated per unit; enters brain in proportion to blood concentration regardless of glucose availability
Brain fuel preference
Research shows brain preferentially uses ketones when both fuels are available (Cahill & Veech, 2003; Cunnane et al.)
Mitochondrial ROS output
Fat-based metabolism produces fewer reactive oxygen species — the primary driver of mitochondrial oxidative damage
What Damages Mitochondria and What Mitochondrial Dysfunction Looks Like
Mitochondrial dysfunction is not a single event. It develops gradually, over years or decades, through accumulated oxidative stress and chronic inflammation. The dietary patterns most strongly associated with this damage are well-documented in the research literature: high intake of refined carbohydrates and added sugars, chronic consumption of ultra-processed foods, and the elevated levels of systemic inflammation those eating patterns produce.
The mechanism is straightforward. High-sugar diets produce chronically elevated blood glucose, which drives excessive ROS generation in mitochondria — particularly in the beta cells of the pancreas, which are under continuous demand for insulin production. These ROS impair mitochondrial membrane integrity, reduce the efficiency of the electron transport chain, and progressively diminish ATP output. A 2021 review in Nutrition and Metabolism (ScienceDirect) documented that ultra-processed diets are associated with measurable increases in systemic oxidative stress markers, decreased antioxidant capacity, and mitochondrial dysfunction.
Ultra-processed foods add an additional layer of damage beyond their macronutrient profile. Many contain advanced glycation end-products (AGEs) — compounds formed when proteins or fats are chemically modified by sugar exposure during processing. AGEs accumulate in tissues and have been shown to directly impair mitochondrial function and accelerate oxidative stress. The food additives present in ultra-processed products — emulsifiers, artificial sweeteners, preservatives — have been identified in recent research as contributors to gut dysbiosis, systemic inflammation, and disruption of cellular energy pathways.
The consequence of all of this is a mitochondrial population that is progressively less capable of meeting the body's energy demands. Cells that should be producing ATP at full capacity are producing it at a fraction of that rate. The body compensates imperfectly: you feel tired, your concentration falters, you crave quick energy from sugar and refined carbohydrates, you eat them, and the cycle accelerates.
Common Signs of Mitochondrial Dysfunction
Persistent fatigue that does not resolve with adequate sleep
Mid-morning and mid-afternoon energy crashes
Fatigue after meals, particularly carbohydrate-heavy ones
Brain fog — difficulty concentrating, slow thinking, word-finding difficulties
Poor sleep quality or waking unrefreshed despite sufficient hours
Cold extremities (hands and feet) — peripheral circulation depends on adequate ATP production
Frequent illness or slow recovery — immune function is energy-intensive
Difficulty losing weight despite dietary changes — impaired fat oxidation is a feature of mitochondrial dysfunction
Low exercise tolerance or prolonged recovery after physical exertion
None of these signs individually diagnoses mitochondrial dysfunction — they overlap with many conditions. But in combination, particularly alongside a diet high in refined carbohydrates and ultra-processed foods, they represent a pattern consistent with impaired cellular energy production. The point is not to alarm; it is to provide a framework for understanding symptoms that are often dismissed as stress, aging, or simply the way things are.
Why High Blood Sugar and Low Energy Keep You Stuck

One of the most frustrating parts of mitochondrial dysfunction is that high blood sugar, low energy, and cravings reinforce each other. The dietary patterns that damage mitochondria also happen to create the conditions that make those same patterns feel necessary and difficult to escape.
Here is how the cycle works. A diet high in refined carbohydrates produces blood glucose spikes followed by rapid drops. When blood glucose drops, the brain signals hunger through the hormone ghrelin, creating a compelling drive to eat — specifically, to eat the quickly digestible carbohydrates that will restore blood glucose fastest. Eating those carbohydrates temporarily resolves the hunger, but generates another spike, another crash, and another hunger signal. The body never stabilizes into a state where it can access stored fat for fuel, because insulin remains chronically elevated — and elevated insulin is a direct suppressor of lipolysis, the process by which fat is released from adipose tissue for energy.
Meanwhile, the mitochondria — damaged by ongoing oxidative stress — produce less ATP per unit of fuel. The body is, in the most literal sense, running on a degraded power supply. Energy output is below what it should be not because the body lacks stored fuel — most people with this pattern have significant stored body fat — but because the metabolic machinery for converting that stored fat to ATP efficiently has been progressively impaired.
I
“The problem is not a shortage of stored energy. It is a dysfunction in the machinery that converts stored energy into usable cellular fuel.”
This is why the standard advice to "eat less and move more" frequently fails people with significant metabolic dysfunction. The issue is not caloric arithmetic; it is a broken energy conversion system. Addressing it requires changing the fuel source, reducing the oxidative load, and giving the mitochondria the conditions they need to begin recovering.
How to Strengthen Your Mitochondria and Support Recovery
The evidence on mitochondrial recovery is encouraging, with one important caveat: the timeline is proportional to the duration and severity of the damage. Mitochondria that have been under chronic oxidative stress for years do not recover in days. The process is gradual, and the improvements — better sleep quality, more stable energy, reduced cravings, clearer thinking — emerge incrementally rather than overnight. Recovery depends on reducing the damage while also giving the body the conditions to build healthier mitochondria.
The most effective interventions are those that reduce the oxidative burden on mitochondria while providing the metabolic conditions that support their recovery and — through a process called mitochondrial biogenesis — the generation of new, healthy mitochondria.
| Intervention | Mechanism and What the Evidence Shows |
|---|---|
| Reduce refined carbohydrates and added sugar | Directly lowers blood glucose variability, reduces ROS production, decreases demand on mitochondrial oxidative phosphorylation, and begins restoring insulin sensitivity. The primary and most impactful first step. |
| Shift toward fat as a fuel source | When carbohydrate intake decreases and insulin drops, glucagon rises and triggers lipolysis — releasing stored fatty acids that the liver converts to ketones. Ketone metabolism produces fewer ROS and more ATP per unit of substrate, reducing mitochondrial oxidative stress with each meal. |
| Eliminate ultra-processed foods | Removes the primary dietary source of AGEs, harmful additives, and industrial seed oils associated with mitochondrial damage and systemic inflammation. Whole, minimally processed foods do not carry these non-nutritive compounds. |
| Time-restricted eating / intermittent fasting | Extending the daily fasting window (typically 12–16 hours) allows insulin to fall, promotes ketogenesis, triggers cellular autophagy — the process by which damaged cellular components including dysfunctional mitochondria are cleared — and supports mitochondrial biogenesis. |
| Exercise — particularly resistance training | Exercise is one of the most potent stimuli for mitochondrial biogenesis. Resistance training and aerobic exercise both upregulate PGC-1α, the primary transcriptional regulator of new mitochondrial production. Skeletal muscle is the largest glucose disposal site in the body and a primary site of mitochondrial density. |
| Sleep quality | Mitochondrial repair and cellular cleanup occur predominantly during sleep. Chronic sleep deprivation impairs mitochondrial function independently of diet. Both sleep duration and sleep quality matter — disrupted sleep architecture limits the repair window available each night. |
The sequence matters. For most people, the most meaningful initial step is dietary — specifically, reducing refined carbohydrates and ultra-processed foods. This single change reduces the primary source of oxidative damage, lowers insulin, begins to shift the body toward fat oxidation, and removes the compounds most directly associated with mitochondrial impairment. The other interventions build on this foundation.
It is also worth being realistic about the timeline. If mitochondrial dysfunction has been developing for years or decades — which, given the prevalence of ultra-processed food consumption in Western diets, is true for a large portion of the adult population — recovery is a process measured in months, not weeks. The body has a remarkable capacity for self-repair when given the right conditions, but that repair takes time. The improvements along the way — better sleep quality emerging in weeks, more stable energy following over months — are meaningful signals that the process is working.
How Mitochondria Affect Metabolism, Insulin Resistance, and Brain Health

Mitochondrial dysfunction does not occur in isolation from other metabolic conditions. It is deeply intertwined with insulin resistance, non-alcoholic fatty liver disease, chronic systemic inflammation, and the cluster of conditions collectively described as metabolic syndrome. In many cases, these conditions share a common upstream cause: chronic dietary patterns that generate oxidative stress, impair cellular energy production, and disrupt the hormonal environment that governs energy storage and release.
Insulin resistance, for instance, both contributes to mitochondrial dysfunction and is exacerbated by it. Impaired mitochondrial function in skeletal muscle — the primary site of glucose disposal — reduces the muscle's ability to take up and use glucose efficiently, which worsens insulin resistance. Insulin resistance, in turn, keeps insulin chronically elevated, which suppresses fat oxidation and maintains the high-glucose metabolic environment that damages mitochondria. The two conditions reinforce each other in a loop that dietary change can interrupt.
The brain is similarly involved. Research on neurodegenerative conditions, particularly Alzheimer's disease, has increasingly framed the disease as one characterized by impaired brain glucose metabolism — neurons that have lost the ability to use glucose efficiently. Ketones, which bypass the glucose metabolism defect, have shown promise in early research as a means of restoring brain energy supply in these conditions. This is not to suggest that mitochondrial dysfunction from dietary choices directly causes Alzheimer's disease; the relationship is complex and multifactorial. But the overlap between the metabolic conditions associated with Western dietary patterns and the metabolic features of neurodegeneration is not coincidental, and it is an active area of serious research.
How to Increase Mitochondria and Restore Your Energy
The goal is not just to feel less tired, but to improve mitochondrial function over time by changing the inputs that shape energy production. The dietary patterns most strongly associated with mitochondrial damage in the research literature are the same patterns that characterize the modern Western diet: high in refined carbohydrates, added sugar, and ultra-processed foods. Reversing the damage begins with reversing those patterns.
WHERE TO START
Step 1 — Remove ultra-processed foods from daily eating. If a product has more ingredients than a whole food would, it is processed. Whole foods do not have ingredient lists.
Step 2 — Reduce refined carbohydrates and added sugar. These are the primary drivers of the glucose spikes and chronic insulin elevation that generate mitochondrial oxidative stress.
Step 3 — Increase healthy fats and protein. These macronutrients produce minimal insulin response, support mitochondrial function, and provide the substrates for ketone production when carbohydrates are low.
Step 4 — Extend the daily fasting window. Even a 12-hour overnight fast allows insulin to fall and creates the hormonal conditions for fat oxidation and cellular repair.
Step 5 — Move. Resistance training and aerobic exercise are among the most potent stimuli for mitochondrial biogenesis — the generation of new, healthy mitochondria.
Step 6 — Protect sleep. Mitochondrial repair happens predominantly during sleep. Both duration and quality matter.
The timeline for recovery is gradual, and that is worth stating clearly. If you have been eating the standard Western diet for years, your mitochondria will not recover in a week. But the direction of change is achievable, and the early markers of improvement — more stable energy between meals, better sleep quality, reduced afternoon fatigue — tend to appear within weeks of meaningful dietary change, well before the deeper metabolic recovery is complete.
Fatigue is not a character trait. It is not inevitable. For a large portion of the people experiencing it chronically, it is a symptom of a specific, identifiable, and addressable metabolic problem. The body has a profound capacity to repair itself when given the right fuel and the right conditions. Understanding the mechanism is the first step toward giving it both.
💡
“You are not broken. Your mitochondria are running on the wrong fuel. Change the fuel, reduce the damage, give your body time — and the energy you have been missing has a way of coming back.”
Key references: Bianconi E et al., "An estimation of the number of cells in the human body" (Annals of Human Biology, 2013); Mookerjee SA et al., "Quantifying intracellular rates of glycolytic and oxidative ATP production and consumption using extracellular flux measurements" (J Biol Chem, 2017); Cahill GF & Veech RL, "Ketoacids? Good medicine?" (Trans Am Clin Climatol Assoc, 2003); Cunnane SC et al., "Can ketones help rescue brain fuel supply in later life?" (Frontiers in Molecular Neuroscience, 2016); PMC7699472 — Castellano CA et al., "Brain glucose and ketone utilization in brain aging and neurodegenerative diseases"; Martínez Leo EE et al., "Ultra-processed diet, systemic oxidative stress, and breach of immunologic tolerance" (Nutrition, 2021); Tristan Asensi M et al., "The impact of ultra-processed foods on cardiovascular diseases and cancer" (ScienceDirect, 2025); Geto Z et al., "Mitochondrial dynamic dysfunction as a main triggering factor for inflammation associated chronic non-communicable diseases" (J Inflammation Research, 2020)..
This article is part of our Gut Health & Recovery series.
Link Here: Gut Health & Recovery
Latest Articles

Calorie Deficit Diet
The calorie deficit model has been the foundation of weight loss advice for over a century. But millions of people follow it precisely...

Insulin Resistance
You don't need a diabetes diagnosis to have insulin resistance. Millions of Americans are living with it right now — tired, foggy...

Type 2 Diabetes
Your A1C is below 6.5%. You're off medication. You feel better than you have in years. So why does your chart still say 'diabetes'?...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
Disclaimer: The information in this article is for educational purposes only and does not constitute medical advice. Fatigue and related symptoms can have many causes, some of which require medical evaluation and treatment. Nothing in this article should be interpreted as a recommendation to change, stop, or start any medication or treatment plan. Always consult a qualified healthcare provider before making significant changes to your diet or lifestyle..
FAQ's
1. How do mitochondria produce energy in the body?
Mitochondria produce energy by converting nutrients such as glucose and fatty acids into ATP through oxidative phosphorylation. This process supplies the energy your cells need for muscle contraction, brain function, hormone signaling, repair, and metabolism. When this process becomes less efficient, fatigue, brain fog, and poor recovery are more likely.
2. What do mitochondria actually do?
Mitochondria are energy-producing structures found in most cells. Their main job is to generate ATP, but they also help regulate fat oxidation, oxidative stress, cellular signaling, and cellular repair. Tissues with high energy demands — like the brain, heart, liver, and muscles — depend heavily on healthy mitochondrial function.
3. What damages mitochondria?
Mitochondria can be damaged by chronic high blood sugar, refined carbohydrates, ultra-processed foods, oxidative stress, chronic inflammation, poor sleep, physical inactivity, and long-term metabolic dysfunction. Over time, these stressors can reduce ATP output and make it harder for the body to burn fat and maintain stable energy.
4. What are the symptoms of mitochondrial dysfunction?
Common signs include persistent fatigue, waking unrefreshed, brain fog, energy crashes after meals, poor exercise tolerance, slow recovery, cold hands and feet, cravings for quick carbs, and difficulty losing weight. These symptoms are not unique to mitochondrial dysfunction, but together they can point to impaired cellular energy production.
5. How do you strengthen mitochondria naturally?
Strengthening mitochondria starts with lowering the metabolic stress that damages them. The most effective steps are reducing refined carbohydrates and added sugar, removing ultra-processed foods, prioritizing protein and whole foods, improving sleep, exercising regularly, and using time-restricted eating when appropriate. These habits support mitochondrial recovery and mitochondrial biogenesis over time.
6. How long does it take to improve mitochondrial health?
Some people notice better energy and fewer crashes within a few weeks, but deeper recovery usually takes longer. Improvements depend on how long metabolic dysfunction has been present, overall diet quality, sleep, movement, and consistency. In many cases, meaningful improvement takes weeks to months rather than days.
Sources
Wallace DC — "A mitochondrial paradigm of metabolic and degenerative diseases" (Science, 2005)
https://pubmed.ncbi.nlm.nih.gov/16306976/
Sivitz WI & Yorek MA — "Mitochondrial dysfunction in diabetes: from molecular mechanisms to functional significance and therapeutic opportunities" (Antioxidants & Redox Signaling, 2010)
https://pubmed.ncbi.nlm.nih.gov/19686046/
Holloszy JO — "Regulation by exercise of skeletal muscle content of mitochondria and GLUT4" (Journal of Physiology and Pharmacology, 2008)
https://pubmed.ncbi.nlm.nih.gov/19109656/
Paoli A et al. — "Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets" (European J Clinical Nutrition, 2013)
https://pubmed.ncbi.nlm.nih.gov/23801097/
Volek JS & Phinney SD — "The Art and Science of Low Carbohydrate Performance" (Beyond Obesity, 2012)

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service

