Edition: Insulin & Blood Sugar
20 March, 2026
In The News
Vol 1, Edition 16
How Insulin Blocks Fat Burning: Fat Storage vs. Fat Burning Explained
Your body is not broken. It is doing exactly what elevated insulin tells it to do — storing fat and refusing to release it. Understanding the insulin switch is the difference between fighting your metabolism and working with it.

Published By: MAP30 Challenge
Authored By: John Shaw
The Fat Switch: Fed State vs. Fasted State
Fat cells locked
HSL enzyme suppressed. Stored fatty acids cannot be released into bloodstream.
Fuel source: glucose
Body burns incoming food for energy. Stored fat remains untouched.
Liver storing glycogen
Excess glucose packaged as glycogen and fat for future use.
Growth hormone suppressed
Fat mobilization and muscle repair hormones are downregulated.
Autophagy off
Cellular repair and cleanup processes are inactive.
Fat cells open
HSL enzyme active. Stored fatty acids released into bloodstream as fuel.
Fuel source: fat + ketones
Liver converts fatty acids to ketones. Brain and muscles run on stored fat.
Liver producing ketones
Fatty acids converted to ketone bodies — efficient, stable fuel for brain and body.
Growth hormone rising
Supports fat mobilization, muscle preservation, and metabolic repair.
Autophagy activating
Cells begin clearing damaged components. Mitochondrial function improves.
The switch between these two states is controlled by one hormone: insulin. Lower insulin = fat burning. Elevated insulin = fat storage. Always.
Most explanations of weight gain treat fat storage as a passive process — an inevitable consequence of eating more than you burn. This framing is incomplete in a way that has cost millions of people decades of failed effort.
Fat storage and fat burning are not two ends of a calorie spectrum. They are two distinct metabolic states governed by a single hormonal switch. That switch is insulin. When insulin is elevated, the body is in fat storage mode — full stop. Fat cells are locked. Stored energy cannot be released. No amount of caloric restriction fully overrides this hormonal instruction.
When insulin is low — genuinely low, not just slightly reduced — the switch flips. Fat cells open. Stored fatty acids are released into the bloodstream. The liver converts them to ketones. The body runs on its own stored energy. This is fat burning mode, and it is the metabolic state that calorie counting alone almost never reliably achieves.
"You cannot burn stored fat and have elevated insulin at the same time. This is not a theory. It is the biochemistry of how adipose tissue works."
How Insulin Controls the Fat Switch
Insulin is released by the pancreas in response to rising blood glucose — primarily from carbohydrate consumption. Its primary job is to move glucose from the bloodstream into cells for energy. But insulin has a second function that is equally important and far less discussed: it is the body's primary fat storage hormone.
Insulin activates an enzyme called lipoprotein lipase (LPL) in fat cells, which promotes the uptake and storage of fatty acids. Simultaneously, insulin suppresses hormone-sensitive lipase (HSL) — the enzyme responsible for releasing stored fat from adipose tissue for use as fuel. While insulin is elevated, HSL is inhibited. Fat cells cannot release their contents. The stored energy is biochemically locked.
Insulin is released by the pancreas in response to rising blood glucose — primarily from carbohydrate consumption. Its primary job is to move glucose from the bloodstream into cells for energy. But insulin has a second function that is equally important and far less discussed: it is the body's primary fat storage hormone.
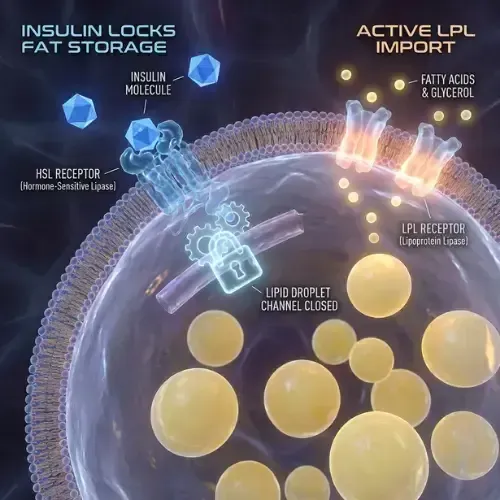
The Two Metabolic States: What Changes When Insulin Falls
| Factor | High Insulin (Fed State) | Low Insulin (Fasted State) |
|---|---|---|
| Fat cell status | Locked — storing fat | Open — releasing fatty acids |
| HSL enzyme | Suppressed — fat cannot exit cells | Active — fat mobilized for fuel |
| Primary fuel source | Glucose from food | Fatty acids and ketones |
| Liver activity | Storing glycogen | Producing ketones from fatty acids |
| Autophagy | Suppressed | Activated — cellular repair begins |
| Growth hormone | Suppressed | Rising — supports fat mobilization |
| Hunger signal | Driven by glucose fluctuations | Stabilizes as fat burning establishes |
🔬 CLINICAL STUDY — Volek JS, Phinney SD et al. (2016)
Nutrition & Metabolism, 13(1), 9.
A controlled dietary intervention comparing low-carbohydrate and high-carbohydrate diets found that subjects on the low-carbohydrate diet — which produced significantly lower insulin levels — showed dramatically higher rates of fat oxidation. Fat burning rates in the low-carbohydrate group were two to three times higher than in the high-carbohydrate group despite similar caloric intake, confirming that the hormonal environment, not caloric balance, is the primary determinant of whether the body burns or stores fat.
What This Means: Lowering insulin through carbohydrate reduction produces fat burning rates 2–3x higher than a high-carbohydrate diet at equivalent calories. The hormonal switch determines metabolic outcome far more than total energy intake.
Why Insulin Resistance Makes Fat Burning Nearly Impossible
In a person with normal insulin sensitivity, insulin rises after eating and falls reliably between meals. The body alternates between fed and fasted states throughout the day, spending meaningful time in fat burning mode even without deliberate fasting.
In a person with insulin resistance, this rhythm breaks down. Cells have become less responsive to insulin's signal, so the pancreas compensates by producing more insulin to achieve the same effect. Fasting insulin — the amount circulating between meals — is chronically elevated. The body rarely, if ever, reaches the insulin nadir required to fully unlock fat burning.
This is why people with insulin resistance can eat less, exercise more, and still fail to lose fat. The caloric math is correct. The hormonal environment is wrong. Elevated fasting insulin means HSL remains partially suppressed around the clock. The fat is there — often in abundance. The body simply cannot access it.
"Insulin resistance is not a weight problem. It is a fuel access problem. The stored energy exists. The hormonal lock prevents the body from reaching it."
🔬 CLINICAL STUDY — Ebbeling CB et al. (2018)
BMJ, 363, k4583.
The CALERIE study and subsequent research by Ebbeling and colleagues at Boston Children's Hospital found that after initial weight loss, subjects who maintained lower insulin levels through reduced carbohydrate intake showed significantly higher energy expenditure than those on high-carbohydrate diets — approximately 250 calories per day more. The authors concluded that the composition of the diet, through its effect on insulin, directly determines how many calories the body burns at rest.
What This Means: The type of food — and its effect on insulin — determines resting metabolic rate after weight loss. Low-insulin dietary approaches do not produce the metabolic slowdown that sabotages calorie restriction. The hormonal environment governs energy expenditure, not just fat storage.
The Metabolic Switch: What It Feels Like When It Flips
The shift from fat storage mode to fat burning mode — what researchers call the metabolic switch — is not an instantaneous event. It follows the depletion of liver glycogen, which typically occurs 10 to 14 hours after the last significant carbohydrate intake. Once glycogen is depleted, the liver begins converting fatty acids into ketones, and fat becomes the body's primary fuel source.
For people who have been in persistent fat storage mode for years — high insulin, low metabolic flexibility, cells conditioned to run on glucose — the transition is often uncomfortable at first. The enzymatic machinery for fat oxidation is downregulated from disuse. The brain resists the shift because it has been dependent on continuous glucose supply.
The symptoms of this transition — fatigue, brain fog, irritability, hunger — are commonly misinterpreted as evidence that the approach is wrong. They are evidence that the switch is flipping, often for the first time in years. They typically resolve within one to two weeks as fat oxidation pathways upregulate and the brain adapts to running on ketones.
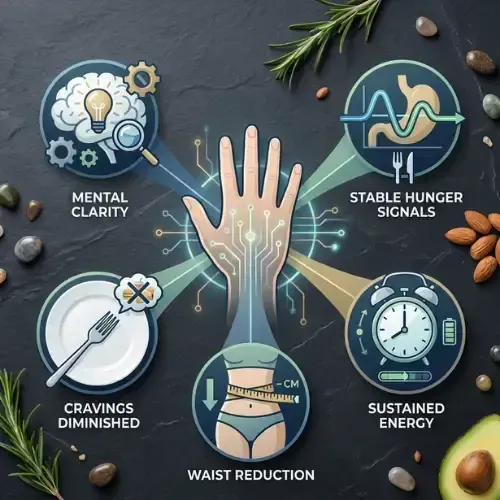
The 5 Signs Your Body Is Burning Fat — Not Sugar:
1. Hunger becomes less urgent and more stable — fat burning provides a steadier fuel supply than glucose spikes
2. Mental clarity improves — the brain functions efficiently on ketones
3. Energy no longer crashes mid-afternoon — no glucose spike means no glucose crash
4. Cravings for sugar and refined carbohydrates diminish — the dopamine-glucose craving cycle weakens
5. Sleep quality often improves — stable blood sugar overnight reduces cortisol disruption.
What Turns the Insulin Switch Off — Unlocking Fat Burning
Fat burning requires insulin to fall. The three most reliable ways to achieve this:
1. Reducing dietary carbohydrate
Carbohydrates produce the largest and most sustained insulin responses of any macronutrient. Reducing refined carbohydrates and added sugars — the highest-insulin-stimulating foods — lowers the insulin baseline more reliably and immediately than any other single dietary change. Protein produces a moderate insulin response. Dietary fat produces almost none.
2. Fasting windows
Every hour without food is an hour of falling insulin. A 12 to 16 hour fasting window — achieved simply by not eating after dinner and delaying breakfast — consistently produces the low insulin nadir required for significant fat oxidation. This is the mechanism behind intermittent fasting's metabolic benefits, covered in depth in the Fasting & Metabolic Reset section of this library.
3. Improving insulin sensitivity
As insulin sensitivity improves — through dietary change, reduced visceral fat, adequate sleep, and resistance exercise — the pancreas needs to produce less insulin to achieve the same glucose management effect. Lower insulin output means lower fasting insulin. Lower fasting insulin means more time in fat burning mode, even without explicit fasting.
These three approaches work synergistically. Reducing carbohydrates lowers the insulin stimulus. Fasting windows extend the low-insulin period. Improving insulin sensitivity reduces the background insulin level that keeps fat storage mode engaged between meals.
Why Calorie Restriction Alone Fails for Fat Loss
This framework explains one of the most frustrating experiences in metabolic health: eating less and exercising more while gaining weight, or losing weight initially and then regaining it despite continuing the same behaviors.
Calorie restriction reduces the total amount of glucose entering the system, which can reduce insulin somewhat. But if the composition of the diet remains high in refined carbohydrates, insulin spikes remain sharp and frequent. Fasting insulin stays elevated. Fat cells remain in storage mode for most of the day. The body compensates for the caloric deficit by reducing energy expenditure — metabolic adaptation — rather than by releasing fat.
The research on metabolic adaptation after caloric restriction is consistent: the body defends its fat stores aggressively when the hormonal environment signals scarcity without the insulin reduction that would permit fat mobilization. The result is weight loss that is heavily skewed toward lean mass — muscle — rather than fat, and a metabolic rate that declines in proportion to the restriction.
Addressing the insulin switch — not just the caloric balance — is what separates fat loss from weight loss.
If you're not sure whether elevated insulin is driving your fat storage pattern, the fasting insulin test identifies the problem years before standard blood work does.
What This Means for the MAP30 Challenge
MAP30 is built around the hormonal conditions required to flip the fat switch. The dietary framework is designed to lower the chronic insulin load that keeps fat cells locked. The fasting protocols create the low-insulin windows in which fat burning activates. The movement framework is calibrated to improve insulin sensitivity directly through muscle glucose uptake — not to 'burn calories.'
If you have tried calorie restriction and failed — if you have eaten less and moved more and watched the scale refuse to move — the answer is not more restriction. It is a different hormonal environment. MAP30 changes the environment first, and fat burning follows from it.
This article is part of our Insulin & Blood Sugar series
Latest Articles
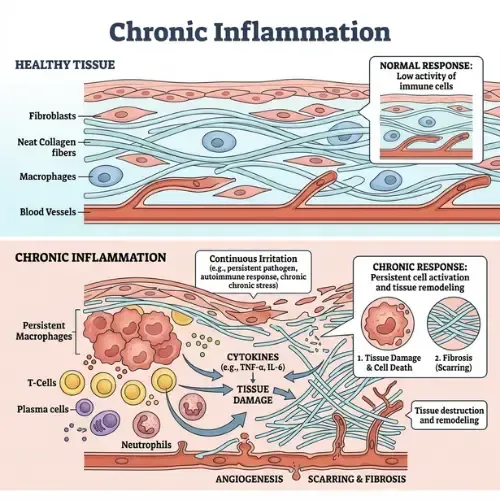
Chronic Inflammation
Chronic inflammation is not the redness and swelling of an injury. It is a silent, systemic biological state that disrupts...

What Is Ghrelin?
Ghrelin is the hormone your stomach sends to your brain when it wants you to eat. Understanding how ghrelin works...

Intermittent Fasting
Most people think fasting is about willpower. The biology tells a different story. When you stop eating, your body doesn't...

John Shaw
MAP30 Challenge
John Shaw is a Certified Nutrition Educator and the founder of the MAP30 Challenge. What began as a personal health journey at 294 pounds, and pre-diabetic, evolved into a structured 30-day metabolic reset program grounded in nutritional science. John's mission is simple: give people the biological education that the diet industry never did.
Disclaimer: The information in this article is for educational purposes only and does not constitute medical advice. Fatigue and related symptoms can have many causes, some of which require medical evaluation and treatment. Nothing in this article should be interpreted as a recommendation to change, stop, or start any medication or treatment plan. Always consult a qualified healthcare provider before making significant changes to your diet or lifestyle..
FAQ's
1. What is the difference between fat storage and fat burning?
Fat storage and fat burning are two distinct metabolic states controlled by insulin. When insulin is elevated — after eating, particularly carbohydrates — fat cells are locked in storage mode and cannot release energy. When insulin falls — during fasting or carbohydrate restriction — the hormonal lock releases, fatty acids flow from fat cells into the bloodstream, and the body burns stored fat for fuel.
2. Why does insulin prevent fat burning?
Insulin activates lipoprotein lipase (LPL) in fat cells, which promotes fat storage, while simultaneously suppressing hormone-sensitive lipase (HSL), the enzyme that releases stored fat for fuel. While insulin is elevated, HSL cannot function normally. Fat is biochemically locked in adipose tissue regardless of caloric intake. This is why people with chronically elevated insulin — a hallmark of insulin resistance — struggle to lose fat even in a caloric deficit.
3. How do I switch my body from fat storage to fat burning mode?
Three approaches reliably lower insulin and activate fat burning: reducing dietary refined carbohydrates and added sugars, which produce the largest insulin responses; extending fasting windows to 12–16 hours, which allows insulin to fall to its nadir; and improving insulin sensitivity through dietary change, adequate sleep, reduced visceral fat, and resistance exercise. These approaches work synergistically — each one makes the others more effective.
4. Why doesn't calorie restriction alone produce fat loss?
Calorie restriction reduces glucose intake but does not necessarily lower the insulin spikes that keep fat cells locked. If the diet remains high in refined carbohydrates, fasting insulin stays elevated, fat cells remain in storage mode, and the body compensates by reducing energy expenditure rather than mobilizing fat. Research shows metabolic adaptation to calorie restriction produces weight loss skewed toward lean mass rather than fat — and a declining metabolic rate that makes continued restriction increasingly difficult.
5. What is the metabolic switch?
The metabolic switch is the transition from burning glucose as the primary fuel to burning fat and ketones — triggered when liver glycogen depletes and insulin falls low enough to allow fat cell release. This typically occurs 10–14 hours into a fast. For people with insulin resistance, the switch is harder to reach because chronically elevated fasting insulin partially suppresses fat mobilization even between meals. Regular fasting windows retrain the body to make this transition efficiently.
6. What are the signs your body is burning fat instead of sugar?
Key signs include: stable hunger without urgent cravings or energy crashes; improved mental clarity and afternoon energy; reduced sugar and carbohydrate cravings; better sleep quality from stable overnight blood sugar; and — over weeks — measurable reductions in waist circumference as visceral fat decreases. These changes reflect the brain and body adapting to fat as a primary fuel, which typically takes one to two weeks of consistent low-insulin conditions to establish.
Sources
Volek JS, Phinney SD et al. — 'Dietary carbohydrate restriction as the first approach in diabetes management' (Nutrition, 2015)
https://pubmed.ncbi.nlm.nih.gov/25287761/
Ebbeling CB et al. — 'Effects of a low carbohydrate diet on energy expenditure during weight loss maintenance' (BMJ, 2018)
https://pubmed.ncbi.nlm.nih.gov/30429127/
Cahill GF — 'Fuel metabolism in starvation' (Annual Review of Nutrition, 2006)
https://pubmed.ncbi.nlm.nih.gov/16848698/
Anton SD et al. — 'Flipping the Metabolic Switch: Understanding and Applying Health Benefits of Fasting' (Obesity, 2018)
https://pubmed.ncbi.nlm.nih.gov/29086496/
Ludwig DS, Ebbeling CB — 'The carbohydrate-insulin model of obesity' (JAMA Internal Medicine, 2018)

Let Me See The Ai Audit Report
I had the MAP30 course material audited and graded by 4 dirrerent Ai models. I was shocked by the grade. See what they had to say about the MAP30 course.

Jaabsha Marketing LLC | All rights reserved 2024 Terms Of Service
